外科病理学实践:诊断过程的初学者指南 | 第13章 肾
第13章 肾(Kidney)
肿瘤(Neoplasms)
The kidney is primarily composed of glomeruli, tubules, stroma, and vasculature. However, unlike in some other organs, the neoplasms of the kidney do not faithfully reflect or recapitulate their cells of origin. Therefore, recognizing a lesion is not so much a systematic process as a pattern recognition. However, there are certain features to notice in evaluating any kidney mass, as they will help narrow the differential diagnosis in tough cases:
肾主要由肾小球、肾小管、间质和脉管系统组成。然而,与其他一些器官不同的是,肾肿瘤不能如实反映或再现其起源细胞。因此,识别病变与其说是一个系统过程,不如说是一个模式识别。然而,在评估任何肾肿块时,都有某些特征需要注意,因为它们有助于缩小困难病例的鉴别诊断范围:
Circumscription and/or encapsulation
边界清楚和/或有包膜
Presence of stroma within the tumor
肿瘤内存在间质
Vascular or capillary pattern
血管或毛细血管模式
Architectural pattern (solid, acinar, trabecular, tubular, papillary, pseudopapillary, cystic)
结构模式(实性、腺泡、小梁、管状、乳头状、假乳头状、囊性)
Cellular pleomorphism (monotonous to bizarre)
细胞多形性(形态单一到奇异形)
Mitotic activity
核分裂活性
Cytoplasm (clear to granular pink to densely eosinophilic; perinuclear halos)
细胞质(透明至颗粒状粉红色至深嗜酸性;核周空晕)
Nuclear size and contour (note the shape and whether the membrane is smooth or wrinkled)
核大小和轮廓(注意核形状,核膜是否光滑或起皱)
Nucleoli
核仁
When studying the kidney grossly, many details crucial to staging are identified (or lost) at the bench. Key prognostic factors include the following:
大体检查时,会获得(或丢失)许多对分期至关重要的细节。关键的预后因素包括:
Tumor extending through the kidney capsule and into the perirenal fat
肿瘤穿透肾被膜延伸至肾周脂肪
Tumor invading adrenal gland (always note whether the adrenal is even present)
肿瘤侵犯肾上腺(始终注意肾上腺是否存在)
Gross tumor in the renal vein, both at the margin and in the renal pelvis (always open the renal vein)
肾静脉内肉眼可见肿瘤(始终打开肾静脉),以及切缘和肾盂肉眼可见肿瘤
Tumor growing through Gerota’s fascia (the very delicate membrane surrounding the peri-renal fat; this is actually fairly uncommon but indicates stage IV disease)
肿瘤生长穿透Gerota筋膜(即肾筋膜;围绕肾周脂肪的非常菲薄的膜;这实际上相当少见,但表明为IV期疾病)
Other helpful gross features include the following:
其他有用的大体特征包括:
Circumscription and presence of multiple lesions
范围和存在多个病灶
If cystic, multilocular versus unilocular, the presence of mural nodules, relationship to pelvis
如果是囊性,观察多房或单房,附壁结节,与肾盂的关系
If solid, the homogeneity and the color(s)—yellow gold, mahogany brown, areas of hemor-rhage, necrosis, fibrosis (gristle grey), or possible sarcomatoid foci (dense white)
如果是实性,观察均质性和颜色(金黄色、红褐色)、出血、坏死、纤维化(软骨灰色)或可能的肉瘤样病灶(致密白色)
Site of origin (cortex vs. medulla or pelvis), if you can tell
起源部位(皮质对比髓质或肾盂),如果你能辨别的话
Now that you have the key identifying features of your tumor, let us look at the differential diagnosis for tumors in the adult.
现在你已经掌握了肿瘤的主要识别特征,让我们来看看成人肿瘤的鉴别诊断。
囊性病变(Cystic Lesions)
单纯性囊肿(Simple Cyst)
Simple cysts are a very common finding, even at autopsy. The simple cyst is essentially a dilated tubule and will have a low cuboidal or flattened pink epithelial lining (Figure 13.1). It is usually unilocular. If multilocular, the septa dividing the cysts should be unremarkable stroma with no epithelial islands or nodules. There should be no clear cells.
单纯性囊肿很常见,甚至在尸检时也是如此。单纯性囊肿实质上是扩张的肾小管,具有低立方形或平坦粉红色的被覆上皮(图13.1)。它通常是单房的。如果是多房性的,分隔囊肿的隔膜应该是不明显的间质,没有上皮岛或结节。应该没有透明细胞。
囊性肾瘤(Cystic Nephroma)
Cystic nephroma is an uncommon lesion, but file it away as “one of those ectopic-ovariantype-lesions in women.” This is a multilocular cyst with a background of ovarian-type stroma (fairly blue, cellular, spindly, and estrogen and progesterone receptor positive; Figure 13.2). The cyst lining is cuboidal to hobnailed. There should be no clear cells.
囊性肾瘤少见,视为“女性异位卵巢型病变”。这是一种多房性囊肿,背景为卵巢型间质(相当蓝,细胞丰富,梭形,ER和PR阳性;图13.2)。囊肿被覆上皮呈立方形至钉状。应该没有透明细胞。
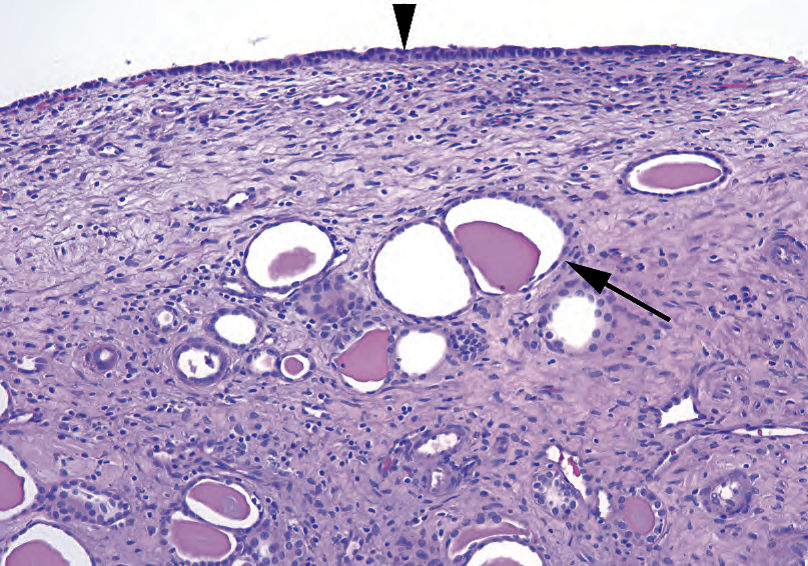
Figure 13.1. Simple cyst. The cyst lining (arrowhead) consists of a thin layer of cuboidal cells. Below the cyst, dilated tubules filled with proteinaceous fluid are visible (arrow).
图13.1.单纯性囊肿。囊肿被覆上皮(箭头)由一层薄薄立方形细胞组成。囊肿下方可见充满蛋白质液体的扩张小管(箭)。
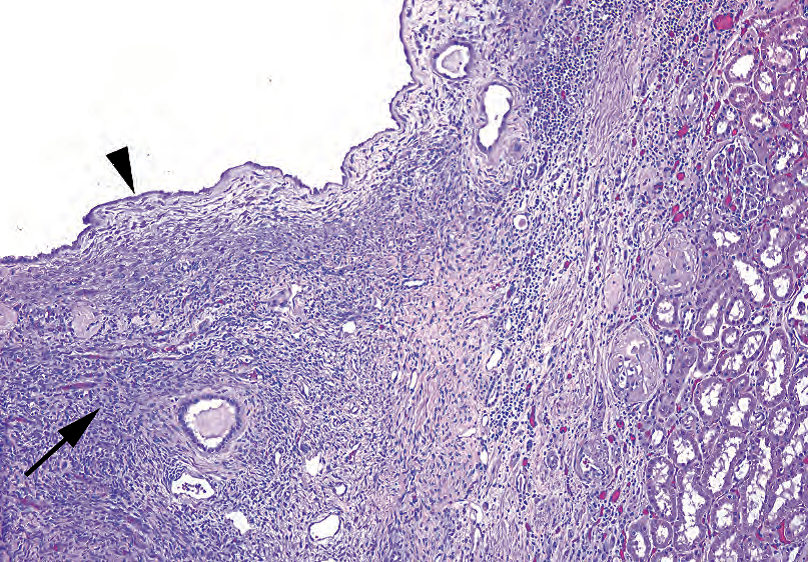
Figure 13.2. Cystic nephroma. Like the simple cyst, this cyst is lined with bland epithelial cells (arrowhead). However, there is adjacent spindly stroma, similar to ovarian stroma (arrow). Kidney parenchyma is seen at right.
图13.2.囊性肾瘤。与单纯囊肿一样,该囊肿内衬形态温和的上皮细胞(箭头)。然而,也有邻近的梭形间质,类似于卵巢间质(箭)。右侧可见肾实质。
混合性上皮-间质肿瘤(Mixed Epithelial-Stromal Tumor)
The mixed epithelial-stromal tumors may be cystic, but are discussed with solid lesions, below.
混合性上皮-间质肿瘤可能是囊性的,下面讨论实体病变。
肾细胞癌(Renal Cell Carcinoma)
Conventional (clear cell) renal cell carcinoma can present as a cyst in several ways. First, it can arise in the wall of a preexisting simple cyst. Second, it can undergo cystic degeneration of a solid tumor. Third, and most sneaky, it can occur purely as a cyst lining, usually in a multilocular cyst: this is called multilocular cystic renal cell carcinoma. The main indicator is the presence of clear cells in the cyst wall (Figure 13.3). The cyst walls may be denuded of epithelium, though, so careful sampling and hunting are essential.
传统的(透明细胞)肾细胞癌可以有多种方式表现为囊肿。首先,它可能发生于先前存在的单纯性囊肿的壁。第二,它可以经历实性肿瘤的囊性变性。第三,也是最隐匿的,它可以是纯粹的囊肿被覆上皮,通常发生在多房囊肿,称为多房囊性肾细胞癌。主要提示线索是囊肿壁存在透明细胞(图13.3)。然而,囊肿壁可能上皮脱落,因此仔细取材和寻找是必要的。
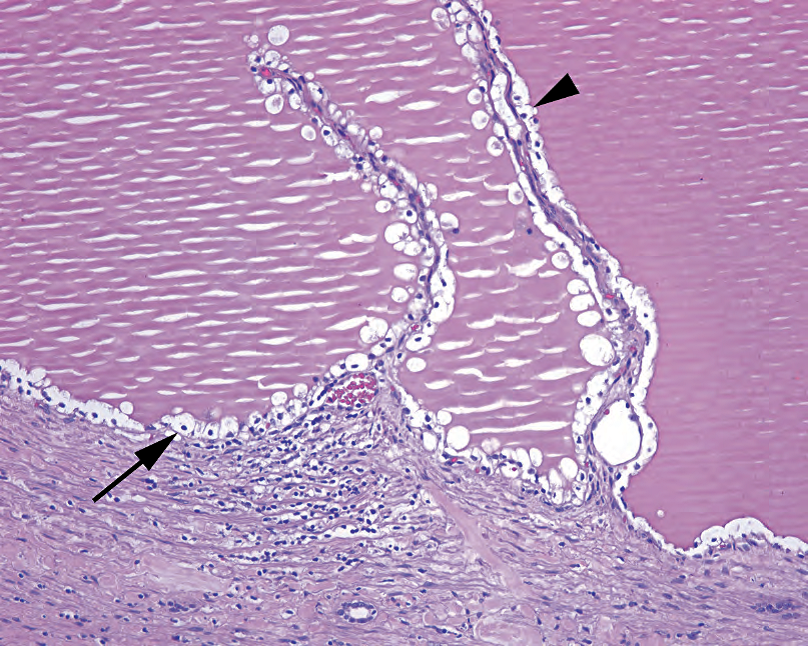
Figure 13.3. Multilocular cystic renal cell carcinoma. The cyst and fibrovascular septa (arrowhead) are lined by single clear cells with small dark nuclei (arrow); compare these cells to conventional renal cell carcinoma (see Figure 13.6).
图13.3.多房囊性肾细胞癌。囊肿和纤维血管间隔(箭头)被覆单层透明细胞,核小而深染(箭);将这些细胞与传统的肾细胞癌进行比较(见图13.6)。
有多种细胞群的病变(Lesions With Multiple Cell Populations)
血管平滑肌脂肪瘤(Angiomyolipoma)
The angiomyolipoma is, at first, a difficult lesion to recognize, because it looks like just a mishmash of normal soft tissue components. From the name, you know that it must have vessels, smooth muscle, and fat, but then so do most organs of the body. Also working against you is the fact that these lesions can have one or two components predominating, so all you see is a mass of plump spindly cells with a vessel here and there, and maybe a couple of fat cells. The key to recognizing an angiomyolipoma is knowing that you have a mass lesion and appreciating the unusual vessels that are the hallmark of this tumor. This tumor is benign. The usual histologic features include the following:
起初,血管平滑肌脂肪瘤是一种难懂的病变,因为它看起来像是正常软组织成分的混杂。从它的名字,你知道它必须有血管、平滑肌和脂肪,但身体的大多数器官也是如此。同样对你不利的是,这些病变可能以一种或两种成分为主,所以你所看到的是一团丰满的梭形细胞,在这里和那里有血管,可能还有一些脂肪细胞。识别血管平滑肌脂肪瘤的关键是存在肿块,并辨认肿瘤特征性不同寻常的血管。这个肿瘤是良性的。常见的组织学特征包括:
Large, tangled, tortuous, thick-walled, hyalinized vessels
大的、缠结的、扭曲的、厚壁的、透明的血管
Smooth muscle cells (pink to clear and spindly) that seem to spin off of, or be continuous with, the vessel walls (Figure 13.4)
平滑肌细胞(粉红色至透明和梭形),似乎从血管壁上脱落或与血管壁相连(图13.4)
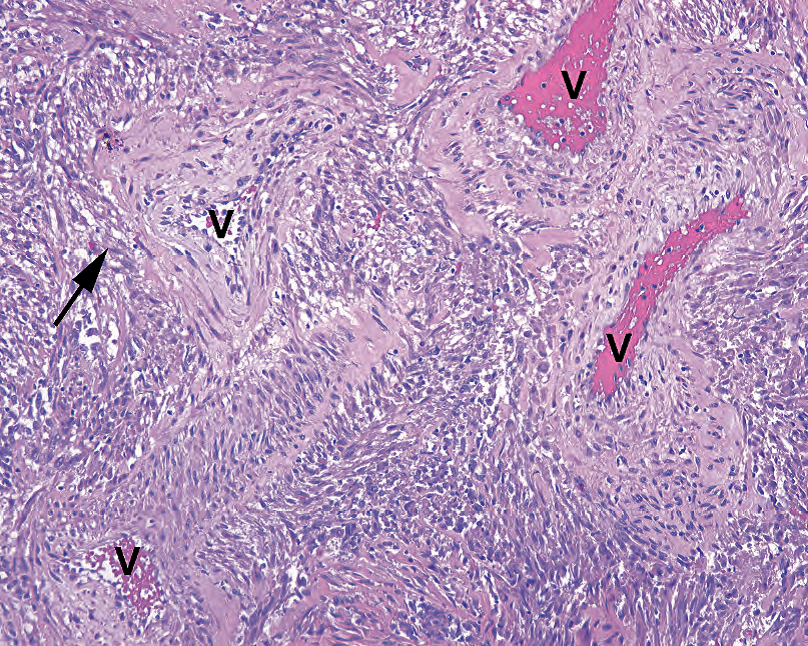
Figure 13.4. Angiomyolipoma. This example does not show the fatty component, but the prominent vessels (V) and smooth muscle components here are classic. In angiomyolipoma, the spindle cells seem to merge with, or spin off from, the thick-walled vessels (arrow).
图13.4.血管平滑肌脂肪瘤。本例未显示脂肪成分,但此处显著的血管(V)和平滑肌成分是经典表现。在血管平滑肌脂肪瘤中,梭形细胞似乎与厚壁血管合并或分离(箭)。
Mature fat cells without atypia or lipoblasts
成熟脂肪细胞,无异型性,无脂母细胞
Pushing borders but not encapsulated
推挤性边界,但无包膜
HMB-45 and Melan-A positive (this tumor is in the perivascular epithelioid cell tumor family, all of which stain for melanoma markers)
HMB-45和Melan-A阳性(该肿瘤属于血管周围上皮样细胞肿瘤家族,均表达黑色素瘤标记物)
混合性上皮-间质肿瘤(Mixed Epithelial-Stromal Tumor)
The mixed epithelial-stromal tumor, although rare, is simple in concept: it is the renal version of an adenofibroma, or a fibroadenoma, or any other benign mixture of stromal and epithelial elements. Because it can be cystic, it is also included in the differential diagnosis of cystic lesions, discussed earlier. The histologic findings include a population of cytologically benign tubules of varying shapes and sizes set in a background of bland spindled stroma, which may consist of smooth muscle, fibroblasts, or myofibroblasts. This may also be in a spectrum with cystic nephroma (discussed earlier), because it also has estrogen receptor– and progesterone receptor–positive stroma.
混合性上皮-间质肿瘤虽然罕见,但概念很简单:它是肾的腺纤维瘤、纤维腺瘤或任何其他间质和上皮成分的良性混合物。因为它可以是囊性的,所以它也包括在囊性病变的鉴别诊断中,前面已经讨论过。组织学发现包括一组不同形状和大小的细胞学良性小管,其背景为形态温和的梭形间质,可能由平滑肌、纤维母细胞或肌纤维母细胞组成。也可能属于囊性肾瘤谱系(前面讨论过),因为它也有ER和PR阳性的间质。
实性肿瘤(Solid Neoplasms)
透明细胞(Clear Cells)
The presence of clear cells in a renal tumor immediately puts renal cell carcinoma at the top of the differential. For all practical purposes, there are no benign clear cell lesions. A 3-mm clear cell focus is still a clear cell carcinoma, albeit a fairly nonthreatening one. Renal cell carcinoma is now understood to have multiple variants, but the clear cell variety is often subtitled “conventional.” Note: Avoid the big, embarrassing, novice mistake number 1—mistaking the normal adrenal cortex for a clear cell tumor. The adrenal clear cell should have visible vacuoles that indent the nucleus, giving it a stellate outline (Figure 13.5).
肾肿瘤出现透明细胞,立即将肾细胞癌置于鉴别诊断的首位。从实用角度,没有良性透明细胞病变。3毫米的透明细胞病灶仍然是透明细胞癌,尽管它没有威胁性。肾细胞癌现有多种变异型,但透明细胞癌常常冠以“传统的”。注意:避免犯第一个大的、令人尴尬的新手错误——将正常肾上腺皮质误认为透明细胞肿瘤。肾上腺透明细胞应有可见的空泡,挤压核,使核呈星芒状轮廓(图13.5)。
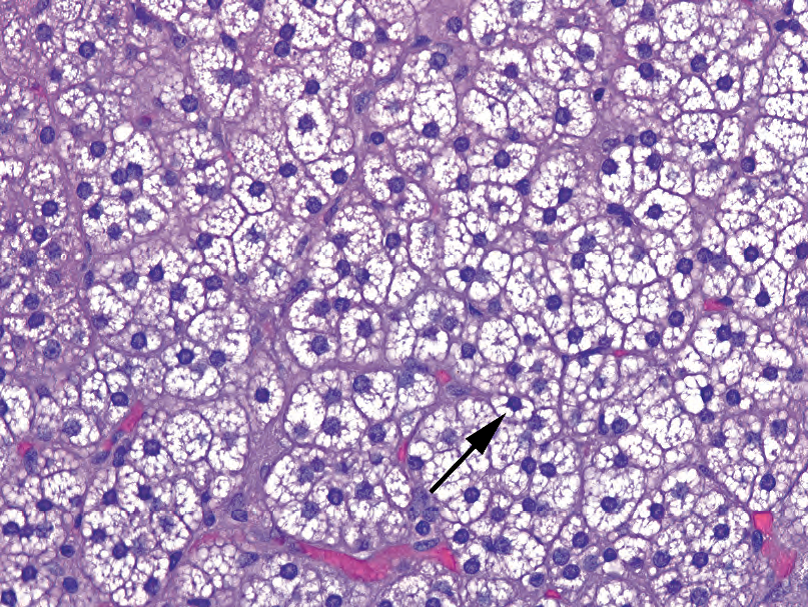
Figure 13.5. Normal adrenal cortex. Unlike clear cell carcinoma, the cells of the adrenal cortex have discrete cytoplasmic vacuoles that indent the nuclei, creating a stellate outline around the nucleus (arrow).
图13.5.正常肾上腺皮质。与透明细胞癌不同,肾上腺皮质细胞有离散的细胞质空泡,挤压核,使核周围形成星芒状轮廓(箭)。
肾细胞癌,传统型或透明细胞型(Renal Cell Carcinoma, Conventional or Clear Cell Type)
Renal cell carcinoma is a common tumor that usually appears grossly as a granular, goldenyellowish-orange, well-circumscribed tumor, looking very much like normal adrenal tissue. It may get quite large and have areas of necrosis, hemorrhage, cystic degeneration, and fibrosis. All different-looking areas should be sampled, especially the firm solid white-to-grey areas, which could indicate sarcomatoid transformation.
肾细胞癌常见,大体表现为颗粒状、金黄色-橙色、边界清楚的肿瘤,很像正常肾上腺组织。它可能体积很大,有坏死、出血、囊性变和纤维化的区域。所有不同外观的区域都应取样,尤其是质硬的实性灰白色区域,这可能提示肉瘤样转化。
Histologically, the tumor may be solid with an acinar pattern, pseudopapillary (which is an acinar pattern with centroacinar dropout), or cystic. Areas of sheeting, spindly, sarcomatoid growth will bump up the tumor to grade IV. Identifying features include the following:
组织学上,肿瘤可为实性伴腺泡、假乳头(腺泡型伴中心腺泡脱落)或囊性模式。成片的梭形肉瘤样生长区域将使肿瘤达到IV级。识别特征包括:
A net-like array of delicate capillaries, dividing cells into packets (“acinar” pattern)
纤细的毛细血管呈网状排列,将细胞分成小团簇(“腺泡”型)
Clear cytoplasm, at least focally if not diffusely (Figure 13.6)
细胞质透明,如果不是弥漫的胞质透明,至少局部如此(图13.6)
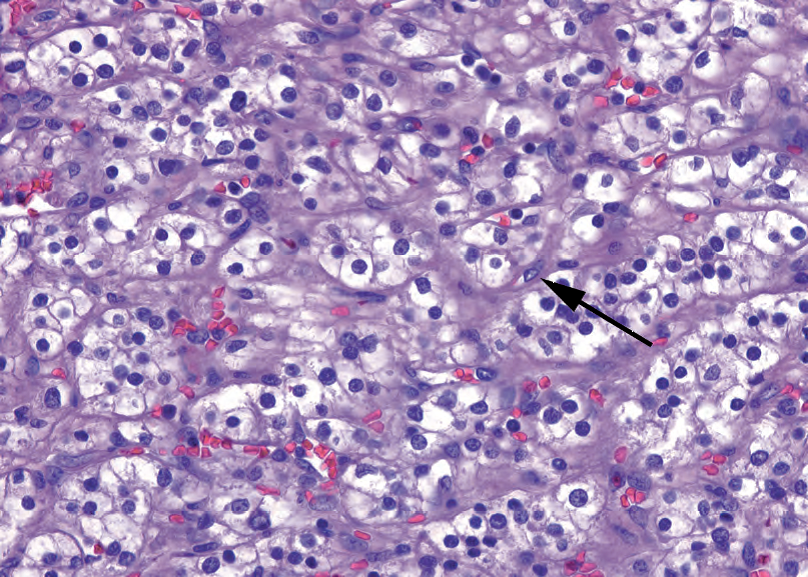
Figure 13.6. Clear cell renal cell carcinoma. The tumor is composed of packets of clear cells, divided by delicate fibrovascular septa (arrow). These septa are characteristic of renal cell carcinoma and are seen even in high-grade or metastatic tumors. The nuclei in this example are enlarged, but nucleoli are visible only at high power, consistent with Fuhrman grade II.
图13.6.透明细胞肾细胞癌。肿瘤由小团簇透明细胞包组成,被纤细的纤维血管间隔分隔(箭)。这些间隔是肾细胞癌的特征,甚至见于高级别或转移性肿瘤。本例中,核增大,但核仁仅在高倍可见,符合Fuhrman II级。
Delicate, distinct cell membranes
纤细、清楚的细胞膜
Lack of desmoplasia (although sclerosis of burned-out tumor is common)
缺乏促结缔组织增生(尽管燃烬的肿瘤继发硬化很常见)
Conventional renal cell carcinoma is graded cytologically according to Fuhrman grade. Lowgrade tumors have clear cytoplasm, polygonal cells, and round nuclei. Higher grade tumors get pink and pleomorphic. Grade criteria, with a 10× objective (Figure 13.7), are as follows:
传统的肾细胞癌根据Fuhrman分级进行细胞学分级。低级别肿瘤有透明胞质、多角形细胞和圆核。高级别肿瘤呈粉红色和多形性。用10×目镜观察,分级标准(图13.7)如下:
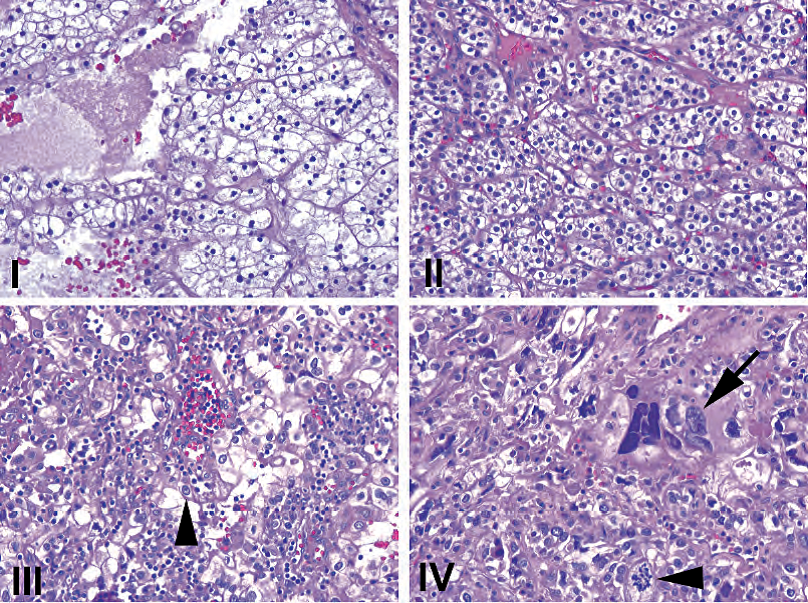
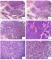
Figure 13.7. Fuhrman grades shown at 10×. (I) Nuclei are small and dense, resembling lymphocyte nuclei. (II) Nuclei are larger, but no nucleoli are visible at this power. (III) Nuclei are even larger, now with some visible nucleoli (arrowhead). (IV) Nuclei are frankly anaplastic (arrow) with large atypical mitoses (arrowhead). All images are taken at the same magnification.
图13.7.10×显示Fuhrman分级。(I)核小而致密,类似淋巴核。(II)核较大,但10×看不到核仁。(III)核更大,现在可见一些核仁(箭头)。(四)核明显间变(箭),伴有大的非典型核分裂象(箭头)。所有图像均为相同的放大倍数。
Grade I: nuclei resemble lymphocytes, no nucleoli (rarely used)
I级:核类似淋巴核,无核仁(很少使用)
Grade II: nuclei still small and without nucleoli, but with open chromatin
II级:核仍然很小,没有核仁,但染色质开放
Grade III: easily recognizable nucleoli, larger nuclei
III级:易于识别的核仁,较大的核
Grade IV: pleomorphic and hyperchromatic nuclei with big nucleoli
Ⅳ级:核多形性、深染,大核仁
肾细胞癌,嫌色变异型(Renal Cell Carcinoma, Chromophobe Variant)
The chromophobe is a carcinoma that has some features of conventional renal cell carcinoma and some features of the oncocytoma. It is, overall, very pale pink under the microscope. It is not encapsulated, and it grows as a solid to papillary mass. Features include the following:
嫌色细胞癌具有传统的肾细胞癌的部分特征,又有嗜酸细胞瘤的部分特征。总体上,在显微镜下呈非常淡的粉红色。无包膜,呈实性至乳头状肿块生长。其特点包括:
Distinct cell membranes that give the tumor a three-dimensional texture, like alligator skin (Figure 13.8)
清楚的细胞膜,使肿瘤像三维结构,如鳄鱼皮(图13.8)
Cells of varying sizes and shapes
不同大小和形状的细胞
Pink, granular, wispy cytoplasm, often with a perinuclear clearing
粉红色,颗粒状,细腻的细胞质,常有核周透明
Nuclei that vary in size and shape and are crinkly, giving a koilocytic look (see Figure 13.8)
核大小和形状不同,呈皱褶状,看似挖空细胞的核(见图13.8)
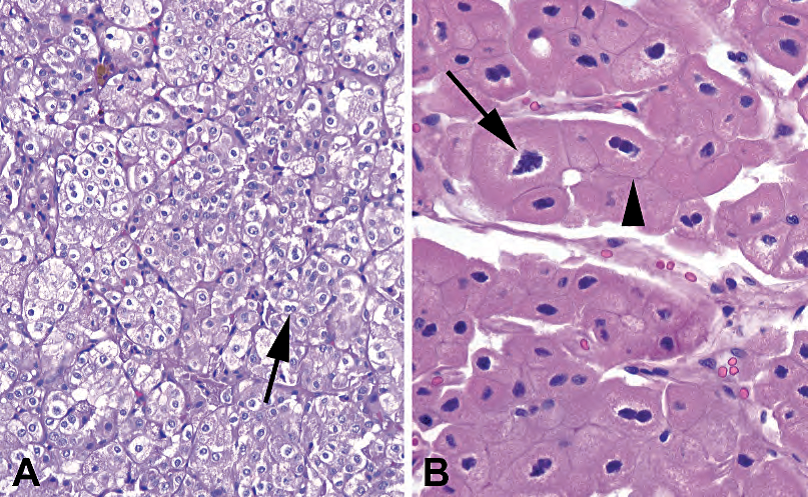
Figure 13.8. Chromophobe carcinoma. (A) Low-power view of a chromophobe, showing packets of cells with clear-to-pink cytoplasm, perinuclear halos, and occasional binucleate cells (arrow). The cell membranes are distinct, giving the tumor a cobblestone or alligator-skin texture. (B) High-power view of a chromophobe carcinoma, eosinophilic variant. Although the granular pink cytoplasm resembles an oncocytoma (see Figure 13.9), the nuclei are distinctly koilocytic, with crinkly outlines and perinuclear halos (arrow). In addition, the crisp cellular membranes are preserved (arrowhead).
图13.8.嫌色细胞癌。(A)低倍,嫌色细胞癌,显示小团簇细胞,细胞质透明至粉红色,核周空晕,偶有双核细胞(箭)。细胞膜清晰,使肿瘤像是鹅卵石或鳄鱼皮的质地。(B)高倍,嫌色细胞癌,嗜酸性变异型。尽管粉红色颗粒性细胞质类似于嗜酸细胞瘤(见图13.9),但核呈明显的挖空细胞样,有皱褶轮廓和核周空晕(箭)。此外,脆弱的细胞膜被保存下来(箭头)。
Cytoplasm positive for Hale’s colloidal iron
Hale胶体铁染色呈阳性的细胞质
Can transform to sarcomatoid morphology
可转化为肉瘤样形态
The eosinophilic variant of chromophobe can look at low power like an oncocytoma, but the nuclei should still have a koilocytic flavor, unlike the very round and regular nuclei of the oncocytoma.
低倍,嗜酸性变异型嫌色细胞癌可能像嗜酸细胞瘤,但核仍应具有挖空细胞的意味,不像嗜酸细胞瘤的非常圆形和规则的核。
粉红色细胞(Pink Cells)
If the cells are not clear, your differential diagnosis includes the following:
如果细胞不透明,你的鉴别诊断包括以下内容:
Chromophobe (discussed above).
嫌色细胞癌(上文讨论)。
High-grade conventional renal cell carcinoma (discussed above).
高级别传统的肾细胞癌(如上所述)。
Oncocytoma: Oncocytoma is a benign tumor resembling oncocytes (or Hurthle cells) in other organs. Grossly, it is mahogany brown and well circumscribed but not encapsulated. There may be a stellate scar (a nonspecific sign of slow growth). The oncocytes are arranged in nests or cords of cells in a hypocellular stroma. The cells are round with dense pink cytoplasm and very regular, round nuclei (Figure 13.9). This regularity should strike you at low power, very different from a chromophobe. The oncocytoma is not graded. Features incompatible with this diagnosis include mitoses, papillary architecture, clear cells, and grossly identified vascular invasion.
嗜酸细胞瘤:一种良性肿瘤,类似于其他器官中的嗜酸细胞(或Hurthle细胞,许特来细胞。译注:正确拼写u上面有两个小点)。大体呈红褐色,边界清楚,但无包膜。可能有星芒状瘢痕(生长缓慢的非特异性迹象)。肿瘤细胞在细胞稀少的间质中排列成巢或条索。细胞呈圆形,胞质深染,呈粉红色,核规则,呈圆形(图13.9)。这种规律在低倍就会让你震撼,与嫌色细胞癌非常不同。嗜酸细胞瘤不分级。不符合本诊断的特征包括核分裂、乳头状结构、透明细胞和肉眼识别的血管浸润。
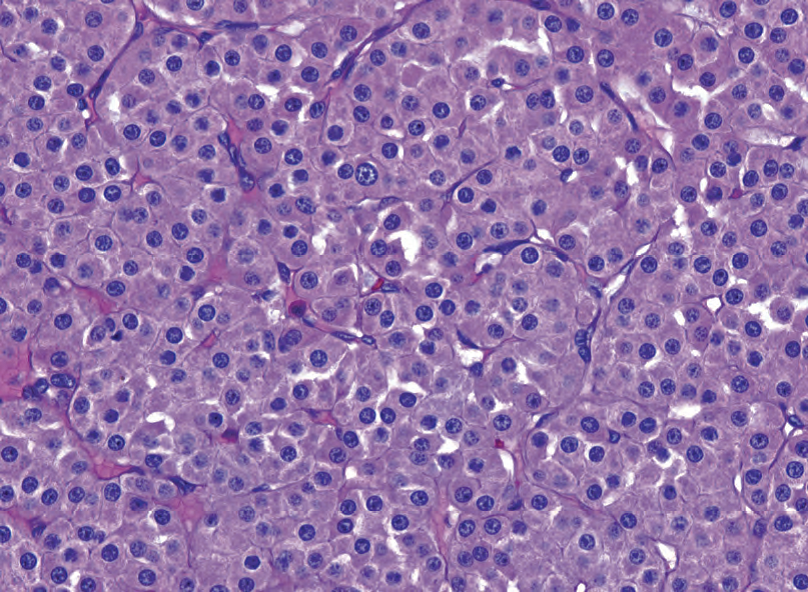
Figure 13.9. Oncocytoma. The nuclei are typically very round, uniform in size, and evenly spaced. Nucleoli may be seen, but there are no perinuclear halos. The cytoplasm is pink and granular, similar to oncocytic neoplasms elsewhere in the body.
图13.9.嗜酸细胞瘤。核通常很圆,大小均匀,分布均匀。可见核仁,但没有核周空晕。细胞质呈粉红色和颗粒状,类似于身体其他部位的嗜酸细胞肿瘤。
Papillary renal cell carcinoma: Papillary renal cell carcinoma is a cellular tumor of pink-to-blue cells (low-nuclear-grade tumors tend to be blue at low power, and high-nuclear-grade tumors tend to be pink; this seems backward) that may be arranged in papillary formations (helpful), solid sheets, or trabecular cords. The classic image is that of a fibrovascular core packed with foamy macrophages and lined by cuboidal cells with round nuclei (Figure 13.10). This image is so pathognomonic that if you find it, you are basically done. You may also see psammoma bodies, hemosiderin-laden cells, and focal clear cells.
乳头状肾细胞癌:由粉红色到蓝色的细胞组成的肿瘤(低核级别肿瘤在低倍镜下呈蓝色,而高核级别肿瘤呈粉红色;这似乎是反常的),可能排列成乳头状结构(有助于诊断)、实性片状或小梁状条索。经典图像为充满泡沫状巨噬细胞的纤维血管轴心,被覆圆核的立方细胞(图13.10)。这种图像如此具有病理诊断意义,如果你找到它,你基本上就确诊了。也可以看到砂粒体、含铁血黄素细胞和局灶性透明细胞。
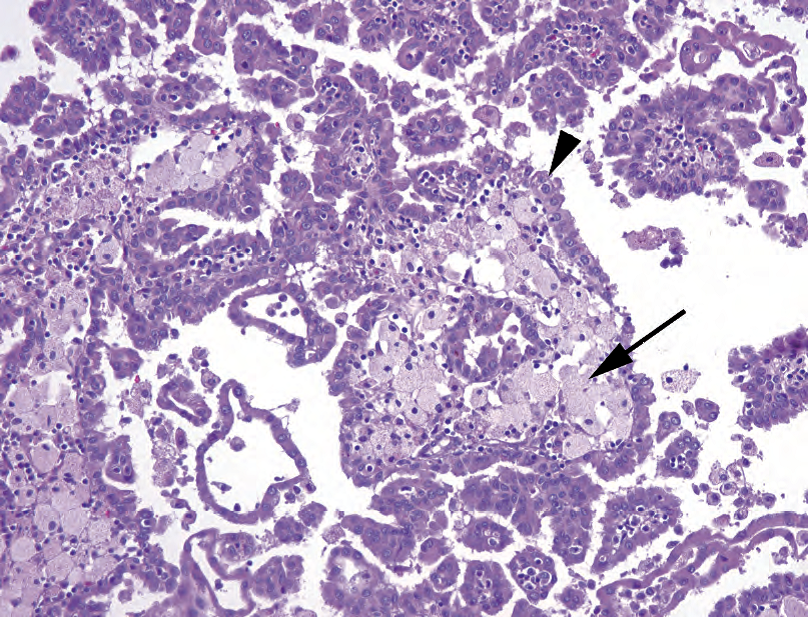
Figure 13.10. Papillary renal cell carcinoma. The tumor cells are eosinophilic, not clear, and range from cuboidal to columnar (arrowhead). This tumor may grow as solid sheets and tubules, but finding papillary structures with central cores packed with foamy histiocytes (arrow) is diagnostic. Although the tumor in this example is low grade cytologically, the cells have a relatively high nuclear/cytoplasmic ratio, and therefore this would be somewhat blue on low power.
图13.10.乳头状肾细胞癌。肿瘤细胞嗜酸性,不透明,从立方形至柱状(箭头)。肿瘤可能以实性片状和小管的形式生长,但发现堆积泡沫状组织细胞的乳头状轴心(箭)具有诊断价值。尽管本例中的肿瘤细胞学级别较低,但核/质比率相对较高,因此在低倍镜下有点呈蓝色。
°Papillary adenoma: By definition, a papillary adenoma is a papillary and non–clear cell neoplasm of low nuclear grade and less than 5 mm in diameter.
°乳头状腺瘤:根据定义,乳头状腺瘤是一种低核级别、直径小于5mm的乳头状非透明细胞肿瘤。
°Xp11: there are several translocation-defined renal cell carcinomas involving the TFE3 gene on Xp11. They occur in young adults. Histologically, they can be summed up as clear cell tumors with papillary architecture.
°Xp11:有几种易位定义的肾细胞癌,涉及Xp11上的TFE3基因。它们发生在年轻成人。组织学,可概括为具有乳头状结构的透明细胞肿瘤。
Collecting duct carcinoma: A collecting duct carcinoma is a high-grade tumor that arises in the medulla. It looks and acts much like an adenocarcinoma. The cytology is clearly malignant, there is a desmoplastic response, and it may stain for mucin and carcinoembryonic antigen. However, it is rare. Rarer still is the variant of collecting duct carcinoma found in sickle cell trait patients, the medullary carcinoma.
集合管癌:发生在髓质的高级别肿瘤。形态学和生物学行为很像腺癌。细胞学明显恶性,有促结缔组织增生反应,黏液染色和CEA染色可能阳性。然而,此癌罕见。在镰状细胞特征的患者中发现的集合管癌变异型,即髓样癌,更为罕见。
蓝细胞(Blue Cells)
When the tumor looks blue, the differential diagnosis includes the following:
当肿瘤呈蓝色时,鉴别诊断包括:
Metanephric adenoma (blue, indigo blue, lymph node blue): Metanephric adenoma is usually a 1x diagnosis. It is a circumscribed but nonencapsulated tumor of monotonous, small, tightly packed, dense blue cells (Figure 13.11). It has little or no cytoplasm. The patterns range from tiny tubules to serpiginous gland-like structures. If this looks like a Wilms’ tumor to you, you are an astute observer. The metanephric adenoma may be essentially a differentiated (mature) form of a pure epithelial Wilms’ tumor.
后肾腺瘤(蓝色、靛蓝、淋巴结蓝色):后肾腺瘤通常为1x诊断(译注:1倍放大,即肉眼观察切片诊断)。它是一种边界清楚但无包膜的肿瘤,由形态单一、体积小、紧密堆积、致密分布的蓝色细胞构成(图13.11)。它几乎没有细胞质。结构模式从小管到蜿蜒的腺样结构不等。如果你觉得它像肾母细胞瘤,你的目光敏锐。后肾腺瘤实质上可能是一种分化(成熟)型纯上皮性肾母细胞瘤。
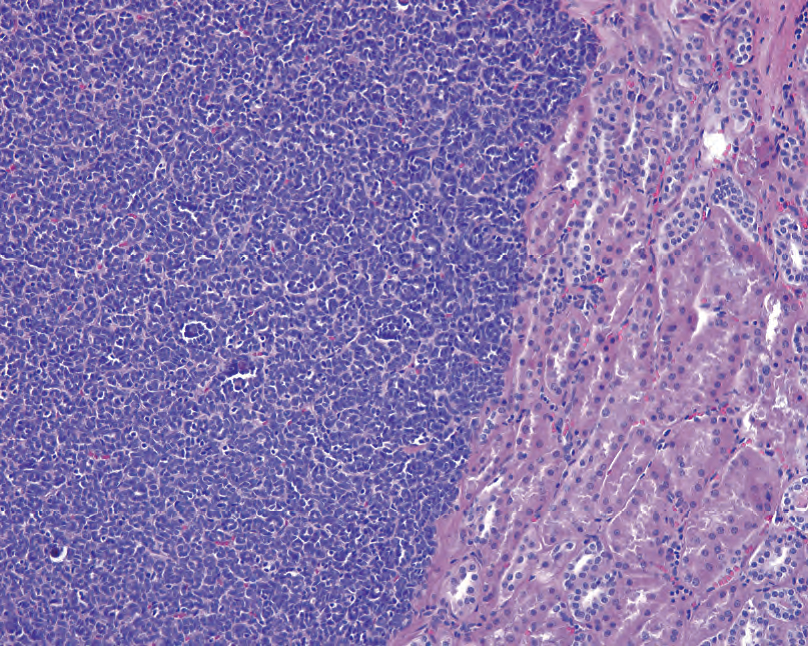
Figure 13.11. Metanephric adenoma. This benign tumor is the bluest of them all because of the very high nuclear/cytoplasmic ratio of the cells. Here you can see tiny primitive blue tubules on the left, adjacent to normal kidney on the right.
图13.11.后肾腺瘤。这种良性肿瘤是所有肿瘤中最蓝的,因为细胞的核/质比非常高。左边可见原始的蓝色小管,邻近右边的正常肾。
Wilms’ tumor: Wilms’ tumors are unusual in adults. See the following discussion of the pediatric population.
肾母细胞瘤:成人少见。参见以下关于儿科肾的讨论。
儿科肾简介(A Brief Introduction to the Pediatric Kidney)
The most common pediatric tumor is Wilms’ tumor, or nephroblastoma, one of the small round blue cell tumors of childhood.
最常见的儿科肿瘤是Wilms瘤,或称肾母细胞瘤,是儿童时期的一种小圆蓝细胞肿瘤。
术语的定义(Definition of Terms)
Nephrogenic rests: abnormally persistent foci of embryonal cells (small, round, and blue) that may develop into Wilms’ tumor, although most do not
肾源性残迹:胚胎细胞(小、圆、蓝)的异常持续病灶,可能发展为肾母细胞瘤,尽管大多数不会
Blastema: sheets of undifferentiated embryonal cells in a Wilms’ tumor, resembling small cell carcinoma
胚芽:肾母细胞瘤中成片的未分化的胚胎细胞,类似小细胞癌
Anaplasia: unfavorable histology in a Wilms’ tumor, defined by large, hyperchromatic nuclei and abnormal mitotic figures (tripolar)
间变:肾母细胞瘤中预后不良的组织学表现,定义为核大深染和异常核分裂象(三级)
肾母细胞瘤(Wilms Tumor)
Wilms’ tumor is defined by triphasic histology, which means you should see three components (Figure 13.12): blastema (undifferentiated, very blue), stroma (generally less cellular, more pink), and epithelium (blue like blastema but organized into tubules). One component may predominate. Histology is defined as favorable or nonfavorable, based on the presence of anaplasia. Finding foci of anaplasia requires extensive sampling and eye-grinding hunting. A Wilms’ tumor may arrive at your bench post-chemotherapy. Chemotherapy changes include massive necrosis, fibrosis, histiocytic replacement, and maturation of the immature elements. One common finding is maturation to skeletal muscle cells.
肾母细胞瘤定义为三相组织学,即,你应该看到三种成分(图13.12):胚芽(未分化,非常蓝),间质(通常细胞较少,较红)和上皮(蓝色像胚芽,但形成小管)。可能以一种成分为主。根据是否存在间变,组织学定义为预后有利或预后不利。需要广泛取材和瞪大眼睛搜索,以发现间变的病灶。可能收到化疗后的肾母细胞瘤标本。化疗的改变包括大量坏死、纤维化、组织细胞取代肿瘤和未成熟成分的成熟。常见发现成熟为横纹肌细胞。
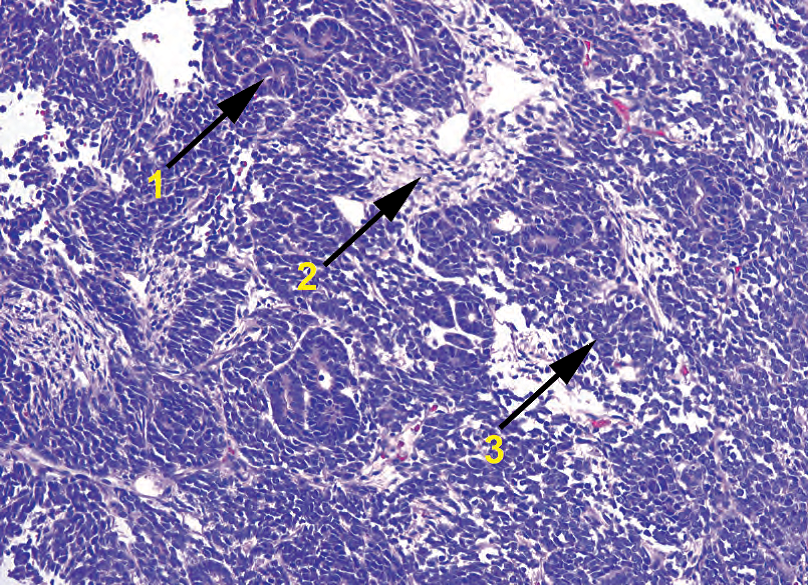
Figure 13.12. Wilms’ tumor. This small round blue cell tumor classically has three components: (1) epithelium, in which the cells form primitive tubules; (2) stroma, the mesenchymal component; and (3) blastema, the most primitive and undifferentiated component. Ratios may vary by tumor.
图13.12.肾母细胞瘤。这种小圆蓝细胞肿瘤典型地由三部分组成:(1)上皮,其中细胞形成原始小管;(2)间质,是间叶成分;(3)胚芽,是最原始和未分化成分。各自比例可能因肿瘤而异。
Wilms’ tumor, like renal cell carcinoma, can grossly resemble a multilocular cyst. This is called a cystic partially differentiated nephroblastoma. The three components are the same.
正如肾细胞癌,肾母细胞瘤大体检查可能类似多房囊肿,称为囊性部分分化性肾母细胞瘤。同样含有三种成分。
其他儿科肿瘤(Other Pediatric Tumors)
Congenital mesoblastic nephroma is a low-grade sarcoma that can resemble fibromatosis (classic type) or fibrosarcoma (cellular type). Metanephric stromal tumor is a spindle cell tumor that infiltrates and entraps native elements such as tubules and blood vessels. Other more aggressive tumors include clear cell sarcoma and rhabdoid tumor. Clear cell nomenclature, which is actually somewhat less than clear, is summarized in the following section.
先天性中胚层肾瘤是一种低级别肉瘤,类似纤维瘤病(经典型)或纤维肉瘤(富细胞型)。后肾间质瘤是一种梭形细胞肿瘤,可浸润并包裹原有成分,如小管和血管。其他浸润性更强的肿瘤包括透明细胞肉瘤和横纹肌样瘤。虽然命名为透明细胞,实际上不太透明,在下一节简述。
关于透明细胞特征的概述(成人和儿童)(A Note on Clear Cell Features, in General (Adults and Children))
You know about clear cell renal cell carcinoma (classically positive for cytokeratins and epithelial membrane antigen [EMA]). Now you also know about the translocation tumors of the kidney, which are clear cells on a papillary core and which arise due to translocations of the TFE3 gene. This same gene can be translocated in the soft tissues, in which case you get alveolar soft part sarcoma(ASPS), which may or may not be clear-cell but does resemble renal cell carcinoma because of its delicate capillary network and alveolar architecture (hence the name). ASPS may be confused with the clear cell sarcoma(CCS) of soft tissue, otherwise known as melanoma of soft parts. Like alveolar soft part sarcoma, it has an alveolar pattern and clear cells; however, it stains for the melanoma markers (S100, Melan-A, and HMB45). This tumor should not be confused with the clear cell sarcoma of kidney, which is totally unrelated to the clear cell sarcoma of soft tissue and is negative for most markers, including S100, cytokeratin, and EMA. However, if you are in the kidney and you have a lesion that is staining for HMB45 and Melan-A, you are most likely looking at an angiomyolipoma, which is a benign tumor having nothing to do with melanocytes but which does stain for the melanoma markers. Is this clear?
你已经知道透明细胞肾细胞癌(典型者呈CK和EMA阳性)。也知道肾的易位性肿瘤,表现为乳头轴心上的透明细胞,病因是TFE3基因易位。软组织也会发生TFE3基因易位,形成腺泡状软组织肉瘤(ASPS),肿瘤细胞可能透明或不透明,但确实很像肾细胞癌,因为二者都有纤细的毛细血管网和腺泡状结构,并因此得名。ASPS可能与软组织的透明细胞肉瘤(CCS)相混淆;软组织CCS也就是软组织的黑色素瘤。与ASPS一样,软组织CCS也有腺泡状结构和透明细胞;然而,软组织CCS表达黑色素瘤标记物(S100、Melan-A和HMB45)。软组织CCS不应与肾CCS混淆,二者完全无关,肾CCS中大多数标记物(包括S100、CK和EMA)均为阴性。然而,如果你在肾发现HMB45和Melan-A阳性的病变,最可能是血管平滑肌脂肪瘤,这是一种良性肿瘤,与黑素细胞无关,但表达黑色素瘤标记物。清楚了吗?
内科肾,非肿瘤(Medical Kidney (Non-neoplastic))
The four main compartments of the nonneoplastic kidney are the glomeruli, the tubules, the interstitium, and the vessels. The compartments are differentially affected by systemic diseases, toxins, and so forth. When evaluating the biopsy, you are looking for the following:
非肿瘤肾观察4种主要成分:肾小球、肾小管、间质和血管。这些成分会受到系统性疾病、毒素等的不同影响。评估活检时,要观察以下各项:
In the glomeruli: the percentage of globally sclerosed glomeruli, hypercellularity (mesangial vs. endocapillary), inflammatory cells, the thickness of mesangial matrix, segmental sclerosis, hyalinosis, crescents, thrombi, and changes in the basement membrane of the capillary loops (especially by PAS and silver stains)
肾小球:总体上硬化肾小球的百分比、细胞增多(系膜对比毛细血管内膜)、炎症细胞、系膜基质的厚度、节段性硬化、透明变性、新月体、血栓和毛细血管袢基底膜的改变(尤其是PAS和银染)
In the tubules: acute and chronic inflammation in the epithelium or lumen, injury (epithe-lial vacuolization, necrosis, or sloughing), cellular or hyaline casts, Tamm-Horsfall protein accumulation, atrophy (dropout)
肾小管:上皮或管腔的急性和慢性炎症、损伤(上皮空泡化、坏死或脱落)、细胞管型或透明管型、Tamm-Horsfall蛋白积累、萎缩(脱落)
In the interstitium: inflammation, fibrosis (especially by trichrome stain), edema
间质:炎症、纤维化(尤其是三色染色)、水肿
In the arteries and arterioles: intimal thickening, hyaline deposits, emboli, thrombotic micro-angiopathy (fibrin thrombi, red blood cell fragments in capillary walls, fibrinoid necrosis)
动脉和小动脉:内膜增厚、透明物质沉积、栓塞、血栓性微血管病(纤维素血栓、毛细血管壁中的红细胞碎片、纤维素样坏死)
This chapter does not go into great detail on these nonneoplastic entities, except to put them into the very big picture.
本章不详细介绍这些非肿瘤实体,只是简述其基本模式。
急性和慢性损害模式(Acute and Chronic Damage Patterns)
肾炎表现(Nephritic Presentations)
Acute injury to the glomerulus (usually immune mediated) leads to a picture of acute glomerulonephritis (hematuria, proteinuria, oliguria, azotemia, edema, hypertension). Histologically, the glomerulus responds with increased cellularity, which includes mesangial cells, endothelial cells, and inflammatory cells. This is a proliferative glomerulonephritis, and in this setting you will also see an interstitial response (edema and inflammation) and red cell casts in the tubules. Causes of this acute injury include postinfectious glomerulonephritis, IgA nephropathy, and lupus.
肾小球急性损伤(通常是免疫介导的)导致急性肾小球肾炎(血尿、蛋白尿、少尿、氮质血症、水肿、高血压)。组织学上,肾小球的反应是细胞增多,包括系膜细胞、内皮细胞和炎症细胞。这是一种增殖性肾小球肾炎,在这种情况下,你还会看到间质反应(水肿和炎症)和肾小管内的红细胞铸型。急性损伤的原因包括感染后肾小球肾炎、IgA肾病和狼疮。
Severe acute injury causes an even more proliferative response in the form of cellular crescents. These are collections of epithelial and inflammatory cells in Bowman’s space, hugging the glomerulus, and they are an indication of severe glomerular injury. You may also see necrosis of the glomeruli, fibrin deposition, and disruption of the basement membrane. Clinically, this appears as a rapidly progressive glomerulonephritis (which is the symptoms of glomerulonephritis plus acute renal failure) and causes include anti–glomerular basement membrane nephropathy (Goodpasture’s syndrome), vasculitis, and anything that can cause a proliferative glomerulonephritis (see above).
严重的急性损伤会导致更严重的增殖反应,形成细胞丰富的新月体。这些是肾小囊间隙中的上皮细胞和炎症细胞的集合,包裹着肾小球,提示严重的肾小球损伤。你还可以看到肾小球坏死、纤维素沉积和基底膜破裂。临床上表现为快速进展性肾小球肾炎(肾小球肾炎加急性肾功能衰竭的症状),病因包括抗肾小球基底膜肾病(Goodpaster综合征)、血管炎以及任何可能导致增殖性肾小球肾炎的疾病(见上文)。
Most of the above diseases are immune-complex mediated, so classification of the location and type of immune complex is key to subclassifying the disease. Immune complexes can be seen by electron microscopy as electron-dense areas, and their location with respect to the basement membrane is important. Immunofluorescence utilizes individual stains for IgG, IgM, IgA, and complement (C1q, C3), and their distribution also helps narrow the diagnosis. Most immune complex diseases have granular immunofluorescence staining, with the exception of anti–glomerular basement membrane disease, which has linear staining of the basement membrane.
上述大多数疾病都是免疫复合物介导的,因此,对免疫复合物的位置和类型进行分类是对疾病进行进一步分类的关键。免疫复合物在电子显微镜下可见,表现为电子密集区,其相对于基底膜的位置很重要。免疫荧光利用IgG、IgM、IgA和补体(C1q、C3)的分别染色,它们的分布也有助于缩小诊断范围。大多数免疫复合物疾病具有颗粒状免疫荧光染色,抗肾小球基底膜疾病例外,该疾病具有基底膜线性染色。
肾病表现(Nephrotic Presentations)
Injury that is limited to the glomerular basement membrane or the podocytes can produce a much more subtle picture. Destruction of the foot processes of the podocytes, which line the basement membrane, or disruption of the basement membrane itself, can lead to a leaky glomerulus that just shows up as proteinuria. Severe proteinuria, and the subsequent edema, hypertension, and so forth, are called the nephrotic syndrome. Diseases in this category include minimal change disease, focal segmental glomerulosclerosis, membranous glomerulonephritis, and membranoproliferative glomerulonephritis. Many other nonprimary renal diseases can also produce this picture, including diabetes, amyloid, lupus, drugs, and infections.
仅限于肾小球基底膜或足细胞的损伤可产生更细微的图像。足细胞的足突(覆于基底膜上)的破坏,或基底膜本身的破坏,均可导致肾小球渗漏,表现为蛋白尿。严重的蛋白尿,以及随后的水肿、高血压等,称为肾病综合征。这类疾病包括微小病变肾病(MCD)、局灶节段性肾小球硬化、膜性肾小球肾炎和膜增殖性肾小球肾炎。许多其他非原发性肾疾病也可以产生这种图像,包括糖尿病、淀粉样蛋白、狼疮、药物和感染。
Of the four primary renal diseases listed earlier, two (minimal change and focal segmental glomerulosclerosis) are not immune complex mediated. They have little or no increase in cellularity and no immunofluorescence findings. You should see evidence of foot process damage by electron microscopy but no deposits. However, membranous and membranoproliferative are immune mediated. Both show thickened and disrupted basement membranes, granular immunofluorescence staining, and ultrastructural deposits. Membranoproliferative glomerulonephritis also has an inflammatory cellular component, so it has an added hypercellular (hyperproliferative ) picture as well as clinical evidence of inflammation (a nephritic picture in addition to the proteinuria).
在前面列出的四种原发性肾病中,有两种(MCD和局灶节段性肾小球硬化)不是免疫复合物介导的。它们的细胞数量几乎不增多或没有增多,并且没有免疫荧光发现。你应该通过电子显微镜看到足突损伤的证据,但没有沉积物。然而,膜性肾小球肾炎和膜增殖性肾小球肾炎是免疫介导的。两者均显示基底膜增厚和破坏,颗粒状免疫荧光染色和超微结构沉积。膜增殖性肾小球肾炎也有炎症细胞成分,因此它也有一个细胞数量增多(增殖)图像以及炎症的临床证据(除了蛋白尿之外的肾炎图像)。
Chronic injury to the kidney produces more of a sclerotic and scarring response, as in other organs. Chronically injured glomeruli become globally sclerotic and look like whorled amorphous pink blobs in the cortex. Chronically injured tubules become flattened, sparse, and dilated, surrounded by interstitial fibrosis and chronic inflammation. When these changes are extensive, you have end-stage kidney and chronic renal failure, and it can be impossible to figure out what the original injury was.
与其他器官一样,肾的慢性损伤会产生较多的硬化和瘢痕反应。慢性损伤的肾小球变得全面硬化,在皮质中看起来像是螺旋状的无定形粉红色斑点。慢性损伤的肾小管变得平坦、稀疏和扩张,周围环绕着间质纤维化和慢性炎症。当这些改变广泛存在,则为终末期肾和慢性肾功能衰竭,可能无法发现最初的伤害是什么。
Most of the diagnoses listed earlier are patterns of injury. While they can be primary renal processes, they can also represent the kidney’s response to systemic diseases. Infection, drugs, and lupus are all examples of systemic diseases that can cause more than one type of kidney damage.
前面列出的大多数诊断都是损伤模式。虽然它们可以是原发性肾疾病,但也可能是肾对系统性疾病的反应。感染、药物和狼疮都可能导致多种肾损害。
Diabetes and hypertension are common, and both are hard on the kidney. Diabetic nephropathy includes thickened basement membranes and increased mesangial matrix; it is not immune complex mediated. The hemodynamic alterations of diabetes also predispose the kidney to glomerulosclerosis, which may be nodular (the Kimmelstiel-Wilson bodies) or eventually global (end-stage kidney disease). Hypertension causes vascular changes in the kidney, including intimal fibrosis of arteries and hyaline deposits in arterioles.
糖尿病和高血压常见,都能对肾造成严重损害。糖尿病肾病包括基底膜增厚和系膜基质增多;它不是免疫复合物介导的。糖尿病的血流动力学改变也使肾易患肾小球硬化症,可能是结节性(Kimmelstiel-Wilson小体)或最终是全面性(终末期肾病)。高血压引起肾的血管改变,包括动脉内膜纤维化和小动脉中的透明物质沉积。
Tubular diseases include acute interstitial nephritis and acute tubular necrosis. Acute interstitial nephritis is reversible damage secondary to drugs and is often associated with eosinophils. Acute tubular necrosis is acute and severe damage to the tubules causing acute renal failure. It may be caused by ischemia or a toxin.
肾小管疾病包括急性间质性肾炎和急性肾小管坏死。急性间质性肾炎是继发于药物的可逆性损害,常伴有嗜酸性粒细胞。急性肾小管坏死是对肾小管的急性和严重损害,导致急性肾功能衰竭。它可能是由缺血或毒素引起的。
Transplant rejection occurs in at least three forms: acute humoral, acute cellular, and chronic. Each form has specific criteria and an associated grading system. The features to look for include the following:
移植排斥反应至少有三种形式:急性体液性、急性细胞性和慢性。每种形式都有特定的标准和相关的分级系统。要查找的特征包括以下内容:
In humoral rejection: glomerulitis, tubular injury, margination of neutrophils, and C4d staining in the peritubular capillaries
体液排斥反应:肾小球炎、肾小管损伤、中性粒细胞边集和管周毛细血管C4d染色
In acute cellular rejection: glomerulitis, interstitial inflammation, tubulitis, and intimal arteritis
急性细胞排斥反应:肾小球炎、间质炎症、小管炎和动脉内膜炎
In chronic rejection: glomerulopathy (double contours in basement membrane), mesangial matrix increase, tubular atrophy, interstitial fibrosis, intimal thickening of arteries, and hyaline thickening of arterioles
慢性排斥反应:肾小球疾病(基底膜双轮廓)、系膜基质增多、肾小管萎缩、间质纤维化、动脉内膜增厚和小动脉透明物质增厚
These types of rejection need to be separated from recurrence of the original disease process, preexisting donor disease (often vascular), and cyclosporine toxicity (tubular injury).
这些类型的排斥反应需要与原有疾病过程的复发、先前存在的供体疾病(通常为血管性)和环孢素中毒(肾小管损伤)相区分。
来源:
The Practice of Surgical Pathology:A Beginner’s Guide to the Diagnostic Process
外科病理学实践:诊断过程的初学者指南
Diana Weedman Molavi, MD, PhD
Sinai Hospital, Baltimore, Maryland
ISBN: 978-0-387-74485-8 e-ISBN: 978-0-387-74486-5
Library of Congress Control Number: 2007932936
© 2008 Springer Science+Business Media, LLC
仅供学习交流,不得用于其他任何途径。如有侵权,请联系删除。
本站欢迎原创文章投稿,来稿一经采用稿酬从优,投稿邮箱tougao@ipathology.com.cn
相关阅读
 数据加载中
数据加载中
我要评论

热点导读
-

淋巴瘤诊断中CD30检测那些事(五)
强子 华夏病理2022-06-02 -
【以例学病】肺结节状淋巴组织增生
华夏病理 华夏病理2022-05-31 -

这不是演习-一例穿刺活检的艰难诊断路
强子 华夏病理2022-05-26 -

黏液性血性胸水一例技术处理及诊断经验分享
华夏病理 华夏病理2022-05-25 -

中老年女性,怎么突发喘气困难?低度恶性纤维/肌纤维母细胞性肉瘤一例
华夏病理 华夏病理2022-05-07







共0条评论