外科病理学实践:诊断过程的初学者指南 | 第8章 结肠
第8章 结肠(Colon)
Colon biopsies are most often performed for one of three reasons:
结肠活检最常见的原因有三种:
1. To evaluate a polyp or mass
1.评估息肉或肿块
2. To study a patient with inflammatory bowel disease and monitor dysplasia
2.对炎症性肠病患者的研究并监测异型增生
3. To look for an explanation for diarrhea
3.寻找腹泻的原因
The history is very important; you should not be diagnosing a tubular adenoma when the endoscopist did not see a polyp. You may also be missing a more ominous diagnosis (discussed later). Assuming that you have at least a succinct history or description from the endoscopist, therefore, your approach to the biopsy depends on what you are looking for.
病史很重要;内镜未见息肉,你就不应该诊断管状腺瘤。如果未知病史,你也可能漏诊更糟糕的病(稍后讨论)。假设你至少获知了简明的病史或内镜医生的描述,因此,你的活检观察方法取决于你在寻找什么。
正常组织学(Normal Histology)
Normal colonic mucosa should have a flat surface and nicely parallel crypts, like “test tubes in a rack.” The crypts are lined with goblet cells, endocrine cells, and precursor cells. Paneth cells, which are red granular cells with basal nuclei, are normal in the ascending and transverse colon but abnormal in the left colon. Immediately under the epithelium is the lamina propria, which is separated from the underlying submucosa by the muscularis mucosa (Figure 8.1). Normal constituents of the lamina propria include lymphocytes, plasma cells, and eosinophils. How many lymphocytes are too many? In general, they are assumed to be physiologic unless there is clinical or histologic evidence of chronic damage to the mucosa (see later discussion). Lymphoid aggregates are common and unremarkable.
正常的结肠粘膜应该有平坦的表面和相当平行的隐窝,就像“架子上的试管”。隐窝被覆杯状细胞、内分泌细胞和前体细胞。Paneth细胞是红色有颗粒的细胞,核位于基底。Paneth细胞在升结肠和横结肠是正常成分,但在左结肠出现时属于异常。紧邻上皮下方的是固有层,由粘膜肌层与粘膜下层分隔(图8.1)。固有层的正常成分包括淋巴细胞、浆细胞和嗜酸性粒细胞。多少淋巴细胞才算太多?一般来说,除非有粘膜慢性损伤的临床或组织学证据(见后面的讨论),否则认为它们是生理性的。淋巴聚集灶是常见现象,没有特殊意义。
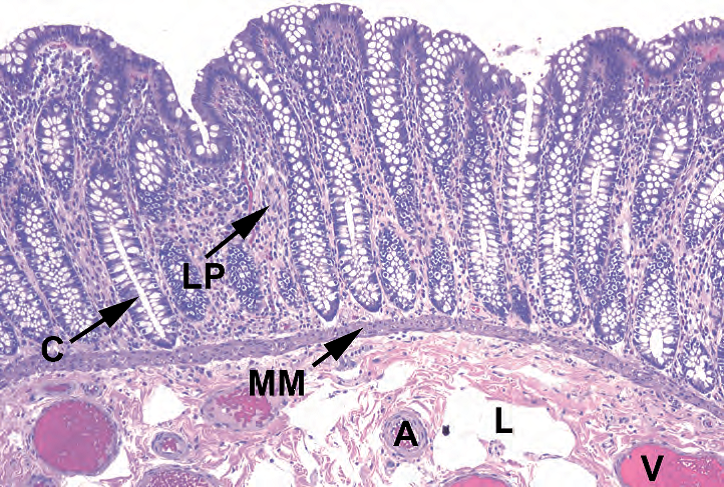
Figure 8.1. Normal colon. Section through colonic mucosa showing parallel crypts (C), lamina propria (LP), muscularis mucosa (MM), and submucosal arteries (A), veins (V), and lymphatics (L).
图8.1.正常结肠。结肠粘膜切片显示平行隐窝(C)、固有层(LP)、粘膜肌层(MM)、粘膜下动脉(A)、静脉(V)和淋巴管(L)。
Deep to the submucosa is the thick muscularis propria. Beyond this layer lies the serosal fat. In biopsy or polypectomy tissue, seeing adipose tissue below the muscularis propria is not normal and means the endoscopist may have taken a full-thickness specimen. In other words, perforated the colon. This should prompt an immediate courtesy call.
粘膜下层的深处是厚厚的固有肌层,再外是浆膜脂肪。在活组织检查或息肉切除组织中,看到固有肌层下方的脂肪组织是不正常的,这意味着内镜检查者可能已经采集了全层标本。换句话说,就是结肠穿孔。应该立即打电话给内镜医生,进行正规的告知。
寻找息肉(Looking for Polyps)
腺瘤(Adenomas)
An adenoma (at least in the tubular-to-villous family) is defined as a polyp with low-grade dysplasia. Low-grade dysplasia in the colon indicates a cytologic change and stands out from normal colon as looking blue on the slide. The cells lining the crypts and the surface become tall and dark (because of depleted mucin) and have cigar-shaped and/or pseudostratified hyperchromatic nuclei (Figure 8.2). Mitoses may be present but are generally not apical.
腺瘤(至少在管状到绒毛状腺瘤家族中)被定义为具有低级别异型增生的息肉状病变。结肠低级别异型增生提示一种细胞学改变,切片看起来呈蓝色,与正常结肠不同。隐窝和表面被覆的细胞变高变深染(由于粘液耗竭),并有雪茄形和/或假复层的深染核(图8.2)。核分裂可能存在,但通常不是位于顶层细胞。
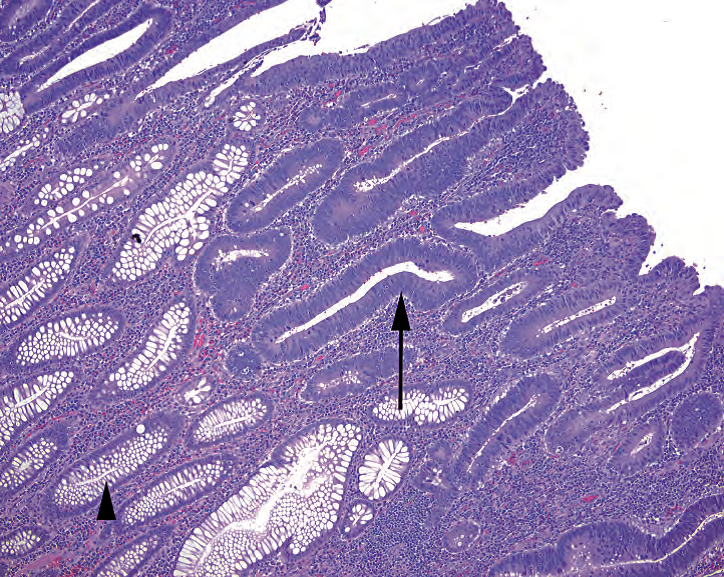
Figure 8.2. Tubular adenoma. This section shows an early tubular adenoma in which low-grade dysplasia is seen in the surface glands (arrow), while the deeper glands are uninvolved (arrowhead). The adenomatous epithelium is dark due to crowded and hyperchromatic nuclei and loss of mucinous goblet cells. Mitotic activity and neutrophils are common in adenomas but may also be seen in benign epithelium.
图8.2.管状腺瘤。切片显示早期管状腺瘤,其表面腺体可见低级别异型增生(箭号),而深层腺体未受累(箭头)。由于核密集深染和失去粘液性杯状细胞,腺瘤的上皮显得深染。腺瘤常见核分裂活性和中性粒细胞,但在良性上皮中也可以看到。
The dysplasia must extend all the way to the surface epithelium to qualify as an adenoma; if the epithelium shows signs of maturing as it ascends, it is more likely reactive changes.
异型增生必须一直延伸到表面上皮,才能称为腺瘤;如果上皮在上升过程中显示出成熟的迹象,更可能是反应性改变。
Adenomas are subdivided by their architecture. The most common type is the tubular adenoma, which has a smooth surface and parallel crypts, similar to normal epithelium. A villous adenoma is covered in finger-like projections, whereas a tubulovillous adenoma has features of both.
腺瘤根据其结构进一步分类。最常见类型是管状腺瘤,表面光滑,隐窝平行,与正常上皮的结构相似。绒毛状腺瘤表面呈手指状突起,而管状绒毛状腺瘤兼有这两种特征。
Important considerations for sign out include the following:
签发报告时重要注意事项包括:
Margins: When an entire polyp is plucked off the colon, ideally it is cross sectioned so that you can see the stalk. Ink on the stalk is helpful, but cautery also identifies your margin. If there are identifiable margins, mention whether or not the dysplasia (adenomatous epithelium) extends to the margin.
切缘:当一个完整的息肉从结肠摘除时,最好沿息肉的长轴包埋并切片,这样你就能看到息肉的蒂。蒂涂抹墨汁是有用的,但烧灼痕迹也能帮助你识别切缘。如果能识别切缘,要说明异型增生(腺瘤性上皮)是否延伸至切缘。
Dysplasia: By definition, low-grade dysplasia is present. However, high-grade dysplasia is equivalent to carcinoma in situ and must be noted. The diagnosis of high-grade dysplasia is made on the basis of architecture rather than cytology. The glands should become cribriform, fused, or back to back (Figure 8.3). Usually the term high-grade dysplasia is reserved for areas that look so complex you are worried about carcinoma but cannot prove invasion. High-grade dysplasia is also usually accompanied by ugly cytology: total loss of nuclear polarity, significant pleomorphism, atypical mitoses, and large nucleoli.
异型增生:根据定义,存在低级别异型增生。然而,高级别异型增生相当于原位癌,必须注意。高级别异型增生的诊断是基于结构而不是细胞学。腺体应变为筛状、融合或背靠背(图8.3)。通常,高级别异型增生这个术语只适用于那些看起来非常复杂的区域,以致你可能会担心癌,但无法证明浸润。高级别异型增生通常伴有丑陋的细胞学表现:核极性完全丧失、显著的多形性、非典型核分裂象和大核仁。
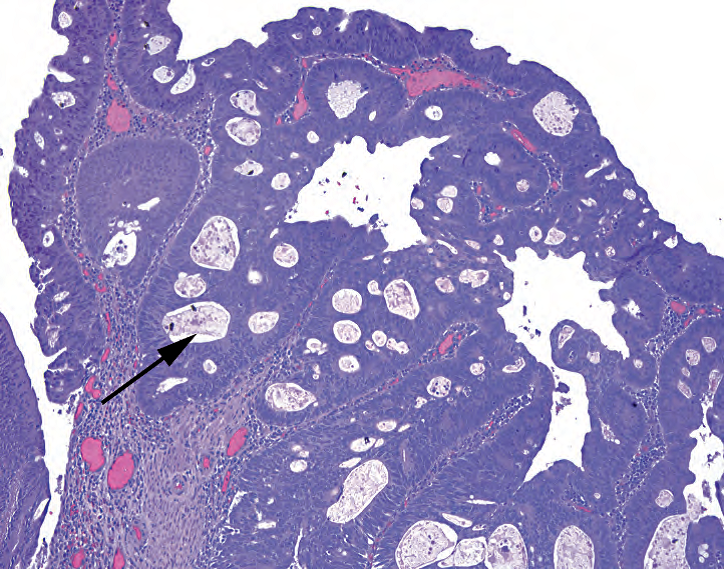
Figure 8.3. High-grade dysplasia in an adenoma. The diagnosis is largely based on architectural features, such as cribriform growth (arrow).
图8.3.腺瘤中的高级别异型增生。诊断主要基于结构特征,如筛状生长(箭号)。
Carcinoma: All adenomas are considered at least premalignant lesions; sometimes you will find carcinoma arising in a polyp on biopsy. To diagnose carcinoma (as opposed to high-grade dysplasia), you must demonstrate cancer crossing the basal lamina, that is, into the lamina propria. Clues to invasion include a jagged interface with the lamina propria, individual infiltrating cells, desmoplastic response, and a pinking up of the invasive cells (Figure 8.4).
癌:所有腺瘤至少认为是癌前病变;有时活检会发现息肉中的癌。要诊断癌(而不是高级别异型增生),必须证实癌穿过基底层,即,进入固有层。浸润的线索包括固有层的界面不规则、呈锯齿状(译注:即基底膜破损)、单个浸润细胞、促结缔组织增生性反应和浸润细胞的变得更红(图8.4)。
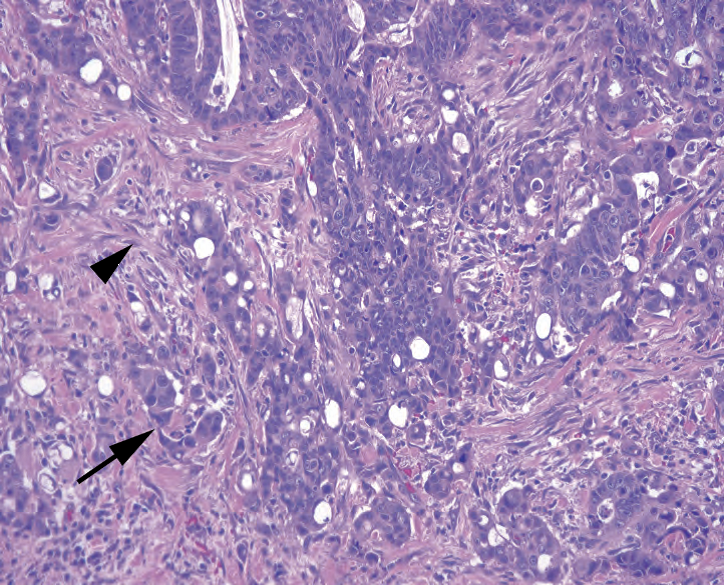
Figure 8.4. Invasive adenocarcinoma. Poorly formed glands and single cells (arrow) infiltrate through a desmoplastic stroma (arrowhead). Cells show marked pleomorphism and prominent nucleoli.
图8.4.浸润性腺癌。形态不完好的腺体和单细胞(箭号)浸润,穿透促结缔组织增生性间质(箭头)。细胞表现出明显的多形性和显著的核仁。
Invasion: Invasion into the lamina propria alone is called intramucosal carcinoma. This may happen in a large polyp, and excision is still curative. Within the lamina propria, cancer has no metastatic potential. However, once malignant cells cross the muscularis mucosa into the submucosa, there is at least theoretical risk of metastasis. The extent of invasion must be noted in the diagnosis.
浸润:仅浸润固有层时,称为粘膜内癌。这种情况可能发生在巨大息肉中,切除仍可能治愈。在固有层内,癌没有转移潜能。然而,一旦恶性细胞穿过粘膜肌层进入粘膜下层,至少在理论上存在转移风险。诊断时必须注意浸润的范围。
(译注:结肠腺癌的定义性特征是癌穿透黏膜肌层并进入黏膜下层。)
增生性息肉(Hyperplastic Polyps)
Hyperplastic polyps are those in which the epithelial cells, although benign, begin to outgrow their available space. The glands have an increased number of goblet cells and therefore look pale or cleared out next to normal epithelium. Furthermore, because the surface area is outgrowing the lamina propria, hyperplastic polyps take on a distinctive frilly (as in a skirt) or lacy appearance (Figure 8.5). Crypts cut in cross section have a distinctive star-shaped lumen.
增生性息肉的上皮细胞虽然是良性,但开始过度生长,超出其可用的空间。腺体中杯状细胞的数量增加,因此在正常上皮旁边看起来深染或透明。此外,由于表面积超过固有层,增生性息肉呈现出独特的褶边(如裙子)或花边外观(图8.5)。隐窝横切面呈独特的星形腺腔。
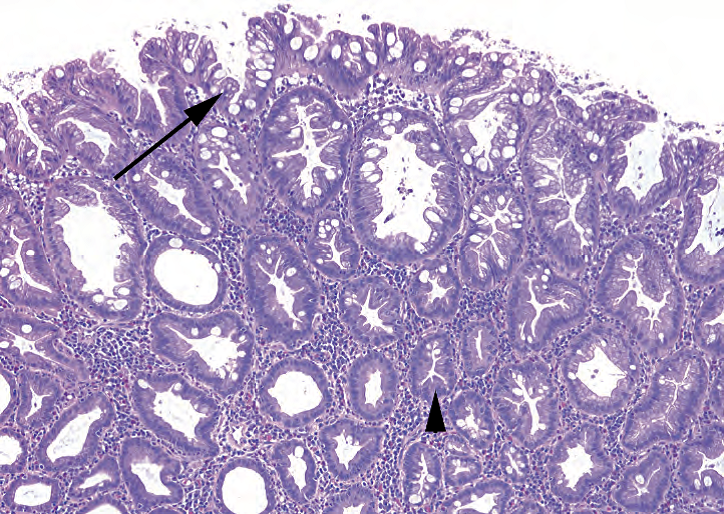
Figure 8.5. Hyperplastic polyp. The surface of the polyp shows a characteristic “frilly” appearance (arrow), with hyperplastic mucinous epithelium and prominent goblet cells. Deeper crypts (arrowhead) show star-shaped lumens.
图8.5.增生性息肉。息肉表面呈典型的“褶边”状(箭号),粘液上皮增生,杯状细胞显著。较深的隐窝(箭头)显示星形腺腔。
A polyp with adenomatous-looking cells at the base of the crypts, and frilly hyperplastic cells at the surface, is still a hyperplastic polyp. Remember that surface maturation is not consistent with a tubular adenoma. However, a true adenoma with a serrated surface profile may be a serrated adenoma (keep reading).
隐窝底部有腺瘤样细胞,表面有皱褶状增生细胞的息肉仍然是增生性息肉。记住,表面成熟不符合管状腺瘤。然而,具有锯齿状表面轮廓的真正腺瘤可能是锯齿状腺瘤(请继续阅读)。
锯齿状息肉(Serrated Polyps)
Serrated is an adjective used to describe the frilly and undulating architecture seen in a classic hyperplastic polyp. Historically, a “serrated adenoma” was a polyp with low-grade dysplasia extending to the surface, as seen in tubular adenoma, but with serrated architecture.
锯齿状是一个形容词,用来描述典型增生性息肉中的皱褶和波浪状结构。历史上,“锯齿状腺瘤”曾用于描述一种息肉状病变,其低级别异型增生延伸至表面,如管状腺瘤所见,但具有锯齿状结构。
Recently, large (>1 cm) hyperplastic polyps occurring in the right colon were recognized as a distinct subtype of polyp with malignant potential, associated with the microsatellite instability (as in hereditary nonpolyposis colorectal cancer [HNPCC]) cancer pathway. They are called either sessile serrated adenomas or sessile serrated polyps. The crypts have characteristic dilation and branching at the base (“duck feet”), and the epithelial cells may be more eosinophilic (less mucin) and pseudostratified than the usual hyperplastic polyp (Figure 8.6). However, mature goblet cells and the frilly surface are still evident.
最近认为,发生在右结肠的大的(>1cm)增生性息肉是一种具有恶性潜能的独特息肉亚型,伴有微卫星不稳定性(正如遗传性非息肉病性结直肠癌[HNPCC])癌症途径。它们称为无蒂锯齿状腺瘤或无蒂锯齿状息肉。隐窝底部有特征性的扩张和分支(“鸭脚”),上皮细胞可能比通常的增生性息肉更红(粘蛋白更少)和假复层(图8.6)。然而,成熟的杯状细胞和皱褶表面仍然很明显。
(译注:sessile serrated adenoma/polyp,无蒂锯齿状腺瘤/息肉,请查阅消化病理专著进一步了解)
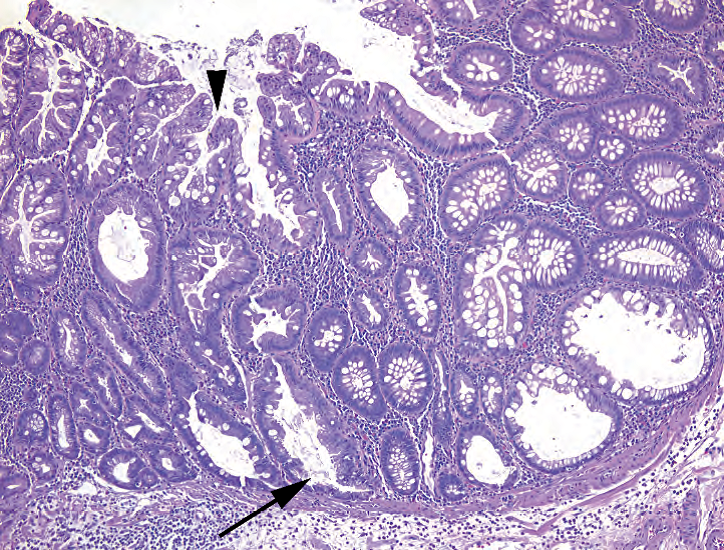
Figure 8.6. Sessile serrated adenoma. The surface looks similar to a hyperplastic polyp (arrowhead), but the base shows sideways branching of crypts (arrow) caused by proliferation at the base of the lesion.
图8.6.无蒂锯齿状腺瘤。表面看起来像增生性息肉(箭头),但底部显示由病变底部增生引起的隐窝侧向分支(箭号)。
The difference is in the depth of proliferation: hyperplastic polyps show mostly surface hyperplasia and expansion, whereas the sessile serrated group (remember that sessile means flat) is hyperplastic right down to the base. These are important to recognize, because they should be treated clinically like an adenoma, not just a hyperplastic polyp.
不同之处在于增殖的深度:增生性息肉主要表现为表面增生和扩张,而无蒂锯齿组(记住无蒂意味着平坦生长)一直增生到底部。认识到这一点很重要,因为它们在临床上应该按腺瘤治疗,而不只是增生性息肉。
炎性假息肉(Inflammatory Pseudopolyps)
Inflammatory pseudopolyps are polypoid structures that consist either of granulation tissue (when adjacent to an ulcer) or of inflamed lamina propria with distorted crypts. Given the inflammation, there can be severe reactive changes in the crypts (resembling dysplasia). However, surface maturation should be visible. These are common in inflammatory bowel disease. A polyp that looks like an inflammatory polyp but occurs without background inflammatory disease may be a juvenile polyp, a diagnosis that can be made in a patient of any age.
炎性假息肉呈现息肉样结构,由肉芽组织(与溃疡相邻时)或发炎的固有层和变形的隐窝组成。既然有炎症,隐窝可能出现严重的反应性改变(类似异型增生)。然而,应当可见表面成熟。这在炎症性肠病中很常见。看似炎性息肉但没有背景炎症,可能是幼年性息肉,可见于任何年龄的患者。
脱垂型病变(Prolapse-Type Lesions)
Mucosal prolapse is like a tiny focus of intussusception; a protruding bulge of mucosa gets pulled, twisted, generally battered in the breeze, suffers ischemia and trauma, and begins to look fairly weird as it tries to repair itself. Features include extension of the muscularis mucosa into the lamina propria, as disorganized fibers; crypt distortion and dilation with diamondshaped crypts; hemosiderin; and edema and inflammation with reactive atypia (Figure 8.7). This lesion may be called a polypoid prolapsing mucosal fold in the colon, solitary rectal ulcer syndrome in the rectum, or inflammatory cloacogenic polyp at the anorectal junction.
粘膜脱垂就像肠套叠的一个微小病灶;粘膜凸起,被牵拉扭曲,在风中凌乱,受缺血创伤,由于试图自我修复,看起来相当怪异。其特征包括粘膜肌层向固有层延伸,形成无序的肌纤维;隐窝变形和扩张,伴有菱形隐窝;含铁血黄素;水肿和炎症伴反应性非典型性(图8.7)。这种病变可称为结肠息肉样脱垂的粘膜皱襞,直肠孤立性直肠溃疡综合征,或肛门直肠交界处炎性泄殖腔息肉。
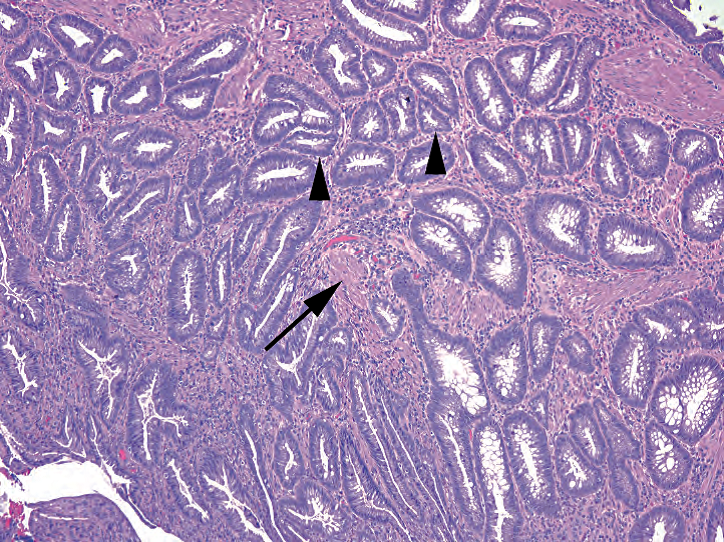
Figure 8.7. Prolapse lesion. The center of this prolapse-related polyp shows typical features, including angulated or diamond-shaped crypts (arrowheads) and smooth muscle growing between crypts (arrow).
图8.7.脱垂性病变。与脱垂相关的息肉的中心显示典型特征,包括成角或菱形的隐窝(箭头)以及隐窝之间生长的平滑肌(箭号)。
腺癌(Adenocarcinoma)
Adenocarcinoma of the colon seems to follow principally two lines of tumorigenesis, highlighted by two familial cancer syndromes. Familial adenomatous polyposis (very rare) is a mutation in the APC gene, a tumor suppressor gene, such that the second allele is vulnerable to somatic mutations. Knockout of both genes leads to adenoma formation. These patients have thousands of tubular adenomas and inevitably progress to adenocarcinoma. p53 is involved in this same pathway, but as a late event in the progression from adenoma to carcinoma. The resulting adenocarcinoma is of the garden variety, indistinguishable from sporadic adenocarcinoma. Approximately 85% of all colon cancers arise from this pathway (most of them sporadic, not familial, hits to these genes).
结肠腺癌似乎主要遵循两种肿瘤发生路线,主要表现为两种家族性癌症综合征。家族性腺瘤性息肉病(FAP,非常罕见)是由于肿瘤抑制基因APC基因发生了突变,因此第二个等位基因容易发生体细胞突变。敲除这两个等位基因导致腺瘤的形成。这些患者有数千个管状腺瘤,不可避免地进展为腺癌。p53也参与这一途径,但在从腺瘤到癌的进展过程中是一个晚期事件。由此产生的腺癌属于普通型,与散发性腺癌难以区分。大约85%的结肠癌是通过这种途径发生的(大多数是散发性,而不是家族性,与这些基因有关)。
The second major pathway is seen in HNPCC patients (less rare), who have defective DNA mismatch repair genes (such as hMLH1 and hMSH2). As above, these are tumor suppressor genes that are vulnerable to the “second hit” somatic mutation. The double hit leads to microsatellite instability. However, instead of tubular adenomas, these tumors tend to arise in the sessile serrated adenomas and mature into medullary, mucinous, or signet-ring cancers, usually right sided. Approximately 15% of all colon cancers fall along this pathway, most of them sporadic.
第二个主要途径见于HNPCC患者(不太罕见),他们有缺陷的DNA错配修复基因(如hMLH1和hMSH2)。如上所述,这些是易受“二次打击”体细胞突变影响的肿瘤抑制基因。双重打击导致微卫星不稳定。然而,这些肿瘤往往发生在无蒂锯齿状腺瘤中,而不是管状腺瘤,并成熟为髓样癌、粘液癌或印戒细胞癌,通常为右侧结肠。大约15%的结肠癌沿这条途径发生,大多数是散发性。
(译注:第二途径即Lynch综合征,LS)
Medullary carcinoma of the colon is a distinct and rare variant with a dense associated lymphoid population (like medullary carcinoma of the breast) but a bland, almost neuroendocrine cytology (like medullary carcinoma of the thyroid), although there is probably no connection. It is worthy of mention in the colon, as medullary carcinoma in the right colon of a young person suggests HNPCC.
结肠髓样癌是一种独特且罕见的变异型,伴有密集的淋巴细胞群(如乳腺髓样癌),但细胞形态温和,类似神经内分泌细胞学(如甲状腺髓质癌),尽管可能与神经内分泌分化无关。结肠发生的髓样癌值得注意,因为年轻人右结肠的髓样癌提示HNPCC。
类癌(神经内分泌)肿瘤(Carcinoid (Neuroendocrine) Tumors)
The most common locations for gastrointestinal carcinoids are the appendix and small bowel, with rectum and colon further down the list. Often submucosal, carcinoid tumors may present as a mass on endoscopy or cause obstruction. The carcinoid syndrome (flushing, etc.) does not occur until and unless the tumor metastasizes to the liver. Carcinoid tumors are characterized by uniform neuroendocrine-type cytology and trabecular, spindly, or rosette-like architecture (Figure 8.8). As in other sites, the histologic features are not predictive of behavior, and a very bland-looking tumor may still metastasize. Neuroendocrine tumors are covered in more depth in Chapter 24.
胃肠道类癌最常见的部位是阑尾和小肠,其次是直肠和结肠。通常粘膜下类癌在内镜下表现为肿块或引起梗阻。除非肿瘤转移到肝脏,否则不会发生类癌综合征(潮红等)。类癌的特征包括均匀一致的神经内分泌型细胞学,以及小梁状、梭形或菊形团样结构(图8.8)。与其他部位一样,组织学特征不能预测行为,形态学非常温和的肿瘤仍可能转移。神经内分泌肿瘤在第24章深入介绍。
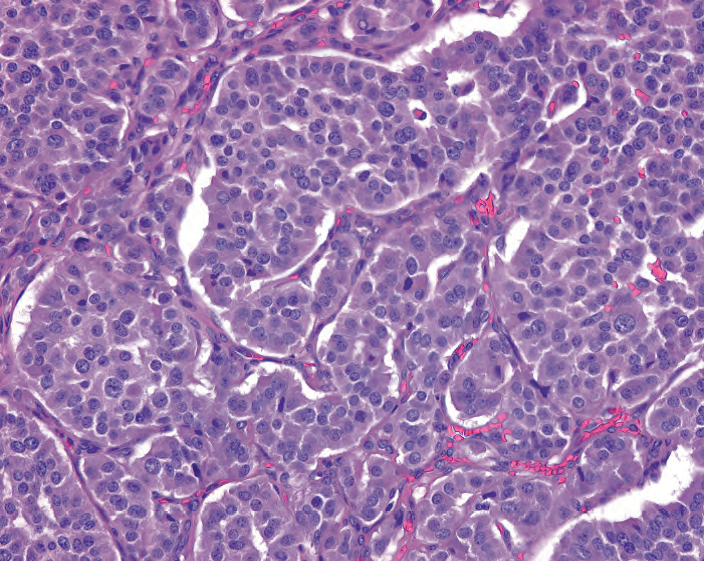
Figure 8.8. Carcinoid tumor. Nests and ribbons of cells separated by delicate fibrovascular septa are classic, as are the round and regular nuclei with finely speckled chromatin.
图8.8.类癌。典型表现为纤细的纤维血管间隔分隔的细胞巢和缎带样结构,细胞学典型表现为圆形和规则的细胞核伴细腻点彩状染色质(椒盐样)。
炎症性肠病(Inflammatory Bowel Disease)
Inflammatory bowel disease (IBD) is an idiopathic relapsing inflammatory disease affecting the colon and consists primarily of ulcerative colitis and Crohn’s disease. A definitive diagnosis of IBD must include changes of chronicity. A simple acute colitis without chronic changes may be due to infection, ischemia, drugs, or bowel preparation, as well as IBD. There is a long list of descriptive diagnoses used for the colon, depending on whether there are acute or chronic changes, whether the changes are focal or diffuse, and whether the patient has a history of IBD. The changes should be pretty compelling to make a first-time diagnosis of IBD, as the patient will carry the label for life.
炎症性肠病(IBD)是一种累及结肠的特发性复发性炎症性疾病,主要包括溃疡性结肠炎和克罗恩病。IBD的确诊必须包括慢性改变。没有慢性改变的单纯急性结肠炎可能由感染、缺血、药物或肠道准备以及IBD引起。结肠有一长串描述性诊断,这取决于是否有急性或慢性改变,改变是局灶性还是弥漫性,以及患者是否有IBD病史。这些改变对于首次诊断IBD应该是非常有说服力的,因为患者将终生带病。
Features of activity (Figure 8.9) include the following:
活动性特征(图8.9)包括以下内容:
Polys, polys, spot the polys: neutrophils in the crypt epithelium = cryptitis.
寻找中性粒细胞,重复三遍:隐窝上皮中的中性粒细胞=隐窝炎。
Neutrophils in the crypt lumen = crypt abscesses.
隐窝腔中的中性粒细胞=隐窝脓肿。
Erosions and ulcers and pus are also consistent with active lesions.
糜烂、溃疡和脓肿也符合活动性病变。
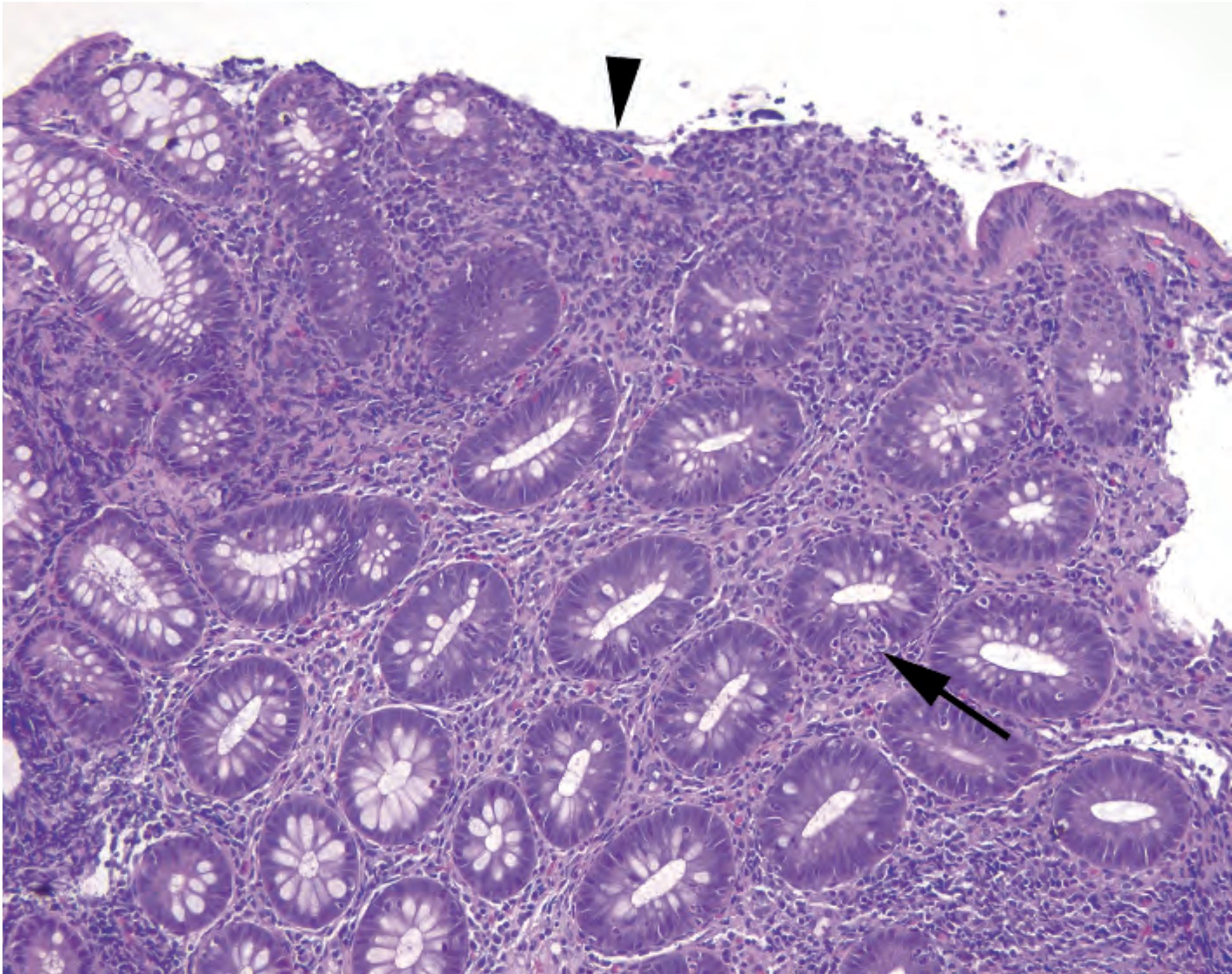
Figure 8.9. Active colitis. Neutrophils are seen in the epithelium of the crypts (arrow), and the surface is ulcerated (arrowhead).
图8.9.活动性结肠炎。隐窝上皮中可见中性粒细胞(箭号),其表面溃疡(箭头)。
Features of chronicity (Figure 8.10) include the following:
慢性特征(图8.10)包括:
Crypt distortion (branching, tortuous, or sideways crypts; test tubes warped)
隐窝扭曲变形(分枝、弯曲或侧向隐窝;试管弯曲)
Crypt loss (test tubes missing)
隐窝丢失(试管丢失)
Crypt atrophy (test tubes too short)
隐窝萎缩(试管太短)
Basal plasmacytosis (test tubes pushed up by a dense layer of chronic inflammation)
基底部浆细胞增多(一层致密的慢性炎症把试管向上推)
Paneth cell metaplasia (Paneth cells in the left colon)
Paneth细胞化生(左结肠Paneth细胞)
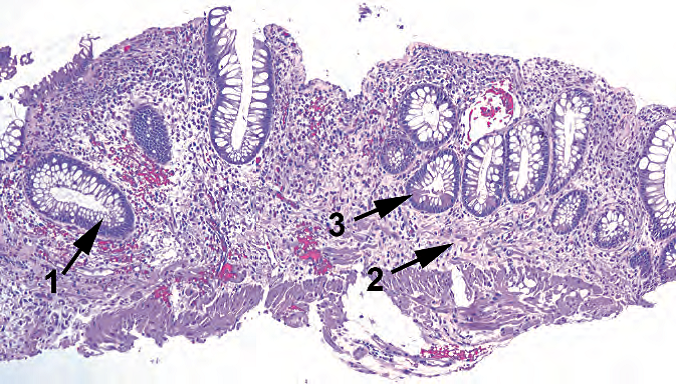
Figure 8.10. Chronic inflammatory disease. This biopsy specimen shows a loss of crypt density (atrophy); crypt distortion (1); elevation of crypts off of the muscularis mucosa (2), often accompanied by a dense basal lymphocytic infiltrate (not seen here); and Paneth cell metaplasia (3).
图8.10.慢性炎症性疾病。活检标本显示隐窝稀疏(萎缩);隐窝扭曲变形(1);粘膜肌层将隐窝抬起(2),常伴有密集的基底部淋巴细胞浸润(此处未见);Paneth细胞化生(3)。
Chronic inflammatory disease is usually qualified as either active (having neutrophils) or inactive. The differentiation between Crohn’s disease and ulcerative colitis is difficult on biopsy; a more definitive diagnosis is made on colectomy (should it come to that). However, there are features that suggest one or the other. Remember that you must first see chronic changes to consider making the diagnosis of IBD (at least at the time of initial diagnosis).
慢性炎症性疾病通常定性并分为活动性(有中性粒细胞)或非活动性。克罗恩病和溃疡性结肠炎在活检标本上难以区分;更明确的诊断是结肠切除术(如果是这样的话)。然而,也有一些特征提示是此或彼。请记住,首先你必须看到慢性改变,才能考虑诊断IBD(至少在初始诊断时)。
克罗恩病的特点(Features of Crohn’s Disease)
Patchy mucosal involvement with skip areas
斑片状粘膜受累伴跳跃区
Granulomas and/or histiocytes (Figure 8.11)
肉芽肿和/或组织细胞(图8.11)
On colectomy, transmural inflammation, cobblestoning, fissures, fistulas, and creeping fat
结肠切除术标本,透壁炎症、鹅卵石、裂缝、瘘管和爬行脂肪
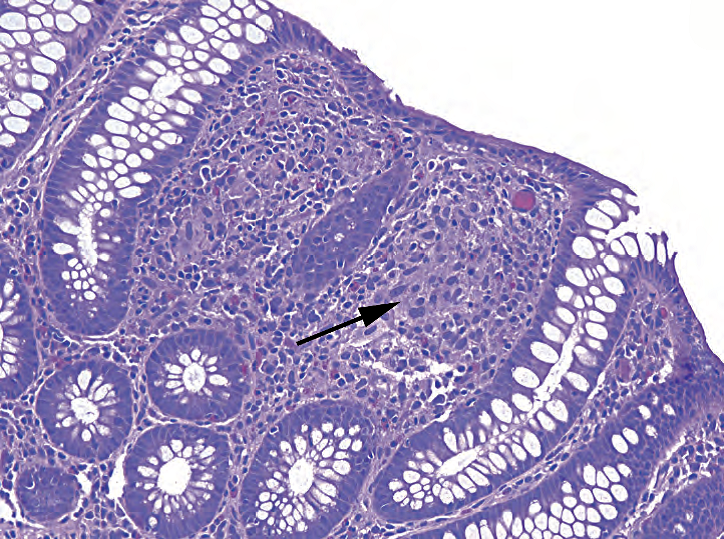
Figure 8.11. Granuloma in Crohn’s disease. The granulomas in Crohn’s are small and subtle. This image, taken at 40×, shows a small collection of histiocytes (arrow) between crypts.
图8.11.克罗恩病的肉芽肿。肉芽肿小而细微。这张40x图像显示隐窝之间的一小团组织细胞(箭号)。
溃疡性结肠炎的特点(Features of Ulcerative Colitis)
Predominantly distal involvement or pancolonic (no skip areas)
主要累及远端结肠或全结肠(无跳跃区)
Diffuse mucosal inflammation, many polys
弥漫性粘膜炎症,多发性息肉
Note, however, that once a patient has begun treatment ulcerative colitis may appear patchy in activity.
然而,请注意,一旦患者开始治疗,溃疡性结肠炎的活动性区域可能会呈现斑片状。
炎症性肠病中的异型增生(Dysplasia in Inflammatory Bowel Disease)
Once diagnosed, IBD must be followed both to monitor activity (response to therapy) and to look for dysplasia. The constant inflammation puts the patient at high risk for developing cancer. Therefore, the presence or absence of dysplasia should be noted in every IBD surveillance biopsy specimen.
一旦诊断IBD,必须随访,观察活动性炎症(对治疗的反应)和寻找异型增生。持续的炎症使患者处于患癌高风险。因此,每个IBD监测活检标本都要注意是否存在异型增生。
The tricky part is that often areas of dysplasia may arise in a polypoid irregularity or fold, and it is difficult to tell a dysplasia-associated lesion or mass (DALM) from a sporadic and unrelated tubular adenoma. Both show the typical adenomatous epithelium. Does it matter? In fact, the DALM may be at higher risk of transforming to cancer and is usually p53 positive on immunostain (unlike an adenoma). It is managed more aggressively than a sporadic adenoma.
棘手的部分是,异型增生区域可能常见于息肉样不规则部位或折叠部位,异型增生相关病变或肿块(DALM)很难与散发性和无关的管状腺瘤相区分。两者均显示典型的腺瘤性上皮。这种区分有意义吗?事实上,DALM可能具有更高的转化为癌症的风险,并且免疫染色通常显示p53阳性(与腺瘤不同)。与散发性腺瘤相比,它的治疗更为积极。
Flat dysplasia (not associated with a mass) can be a subtle and subjective call. Intense inflammation causes reactive changes that can look much like dysplasia. However, remember that true dysplasia does not mature at the surface. Also, be very wary of calling dysplasia in a sea of neutrophils.
平坦型异型增生(不伴肿块)可能是一种微妙的主观的称呼。强烈的炎症引起反应性改变,可能看起来很像异型增生。然而,请记住,真正的异型增生在表面并不成熟。另外,在嗜中性粒细胞的海洋中,不要轻易地称为异型增生。
显微镜下结肠炎(Microscopic Colidities)
Microscopic colidities are defined by having no abnormal endoscopic findings; they are only diagnosable under the microscope. The symptoms include chronic watery diarrhea, abdominal pain, fatigue, and weight loss. The two types are lymphocytic colitis and collagenous colitis. Both are characterized by the following:
显微镜下结肠炎的定义为没有异常的内镜检查结果;它们只能在显微镜下诊断。症状包括慢性水样腹泻、腹痛、疲劳和体重减轻。有两种类型,即淋巴细胞性结肠炎和胶原性结肠炎。两者的特点如下:
A lack of chronic changes (no crypt distortion, no basal plasmacytosis)
缺乏慢性改变(无隐窝扭曲变形,无基底部浆细胞增多)
A predominantly top-heavy lymphocytic infiltrate
主要是顶部重度淋巴细胞浸润
Intraepithelial lymphocytes
上皮内淋巴细胞
Evidence of damage to the epithelium (loss of cells)
上皮损伤的证据(细胞丢失)
Collagenous colitis affects predominantly women and has a distinct thickened collagen band along the basement membrane. This band must be irregular and blurred into the lamina propria, not just thick. A trichrome stain confirms the diagnosis (Figure 8.12).
胶原性结肠炎主要影响女性,基底膜有明显增厚的胶原带。这条带子必须是不规则的,模糊地融入固有层,而不仅仅是增厚。三色染色证实诊断(图8.12)。
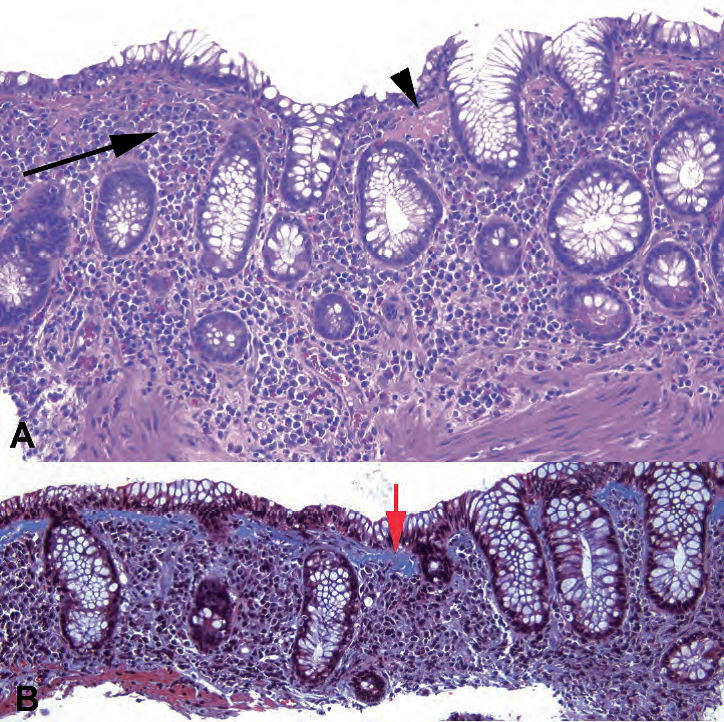
Figure 8.12. Collagenous colitis. (A) The hematoxylin and eosin stain shows a top-heavy lymphoplasmacytic infiltrate (arrow) accompanied by a dense pink material just under the surface epithelium (arrowhead). (B) A trichrome stain confirms the thickened collagen table (blue on this stain, red arrow), which has an irregular border and entraps nuclei within the lamina propria.
图8.12.胶原性结肠炎。(A)HE染色显示顶部重度淋巴细胞浆细胞浸润(箭号),表面上皮下有致密的粉红色物质(箭头)。(B)三色染色证实增厚的胶原带(染为蓝色,红色箭头),其边界不规则,并将细胞核陷在固有层内。
In the setting of a dense lymphoplasmacytic infiltrate, pay attention to whether the blueness is top heavy (more prominent under the surface) or bottom-heavy (more prominent at the base of the crypts). Inflammatory bowel disease tends to be bottom-heavy and the microscopic colidities more top-heavy. This is a soft feature rather than a rule.
在密集的淋巴浆细胞浸润的情况下,注意蓝色是顶部重度(表面下方更显著)还是底部重度(隐窝基底部更显著)。炎症性肠病倾向于基底部重度,而显微镜下结肠炎倾向于顶部重度。这是一个软特性,而不是规则。
其他结肠炎(Other Colidities)
Ischemic colitis may have many appearances, from focal active colitis to diffuse pseudomembranous colitis. Acute or transient ischemia appears as damage to the superficial surface of the mucosa, with hemorrhage and coagulative necrosis. Prolonged ischemia causes fibrosis of the lamina propria and a top-down atrophy of the crypts: they appear collapsed at the surface and regenerative at the base (Figure 8.13).
缺血性结肠炎可能有许多表现,从局灶性活动性结肠炎到弥漫性假膜性结肠炎。急性或暂时性缺血表现为粘膜表面损伤,伴有出血和凝固性坏死。长期缺血导致固有层纤维化和隐窝自上而下萎缩:表面塌陷,底部再生(图8.13)。
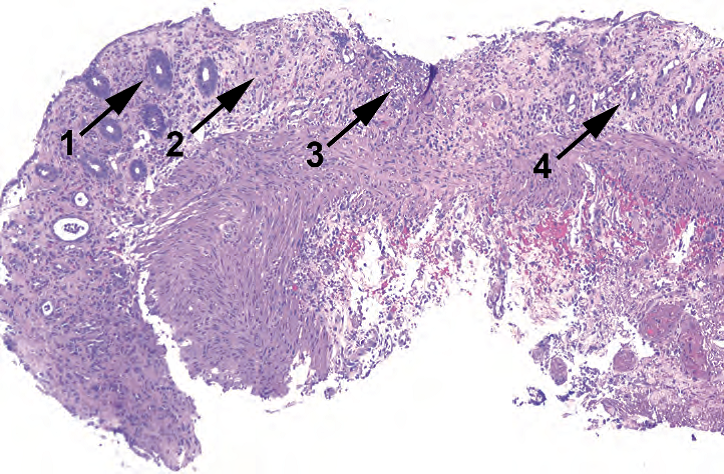
Figure 8.13. Ischemic colitis. Features include small dark regenerative crypts (1), hyalinization and fibrosis of the lamina propria (2), ulceration (3), and crypt dropout (4).
图8.13.缺血性结肠炎。特征包括小而深染的再生隐窝(1)、固有层透明变性和纤维化(2)、溃疡(3)和隐窝脱落(4)。
Infectious colitis is not often biopsied because of its usually self-limited course. It may range from no pathologic findings to a severe active colitis.
感染性结肠炎不常活检,因为通常自愈。其范围从没有病理发现到严重的活动性结肠炎。
Diversion colitis is a special entity associated with a Hartmann pouch, which is a blindended rectal cavity disconnected from the fecal stream. The loss of normal colonizing flora causes a nonspecific colitis, which may be mistaken for inflammatory bowel disease.
改造(或分流)性结肠炎是一种与Hartmann囊相关的特殊疾病,Hartmann囊是一种与粪便流不相连的盲端直肠腔。失去正常菌群会导致非特异性结肠炎,可能误认为炎症性肠病。
Both drugs and the bowel preparation process may cause transient acute colitis. Acute inflammation in the absence of chronic changes is non-speficic, and should not be overinterpreted.
药物和肠道准备过程都可能导致暂时性急性结肠炎。无慢性改变的急性炎症属于非特异性炎症,不要过诊断。
来源:
The Practice of Surgical Pathology:A Beginner’s Guide to the Diagnostic Process
外科病理学实践:诊断过程的初学者指南
Diana Weedman Molavi, MD, PhD
Sinai Hospital, Baltimore, Maryland
ISBN: 978-0-387-74485-8 e-ISBN: 978-0-387-74486-5
Library of Congress Control Number: 2007932936
© 2008 Springer Science+Business Media, LLC
仅供学习交流,不得用于其他任何途径。如有侵权,请联系删除。
本站欢迎原创文章投稿,来稿一经采用稿酬从优,投稿邮箱tougao@ipathology.com.cn
相关阅读
 数据加载中
数据加载中
我要评论

热点导读
-

淋巴瘤诊断中CD30检测那些事(五)
强子 华夏病理2022-06-02 -
【以例学病】肺结节状淋巴组织增生
华夏病理 华夏病理2022-05-31 -

这不是演习-一例穿刺活检的艰难诊断路
强子 华夏病理2022-05-26 -

黏液性血性胸水一例技术处理及诊断经验分享
华夏病理 华夏病理2022-05-25 -

中老年女性,怎么突发喘气困难?低度恶性纤维/肌纤维母细胞性肉瘤一例
华夏病理 华夏病理2022-05-07







共0条评论